Get Care
Hiatus Hernia
What is a Hiatus Hernia?
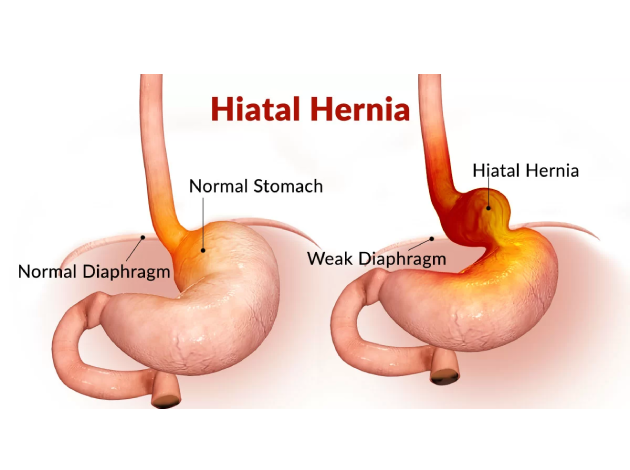
A hiatus hernia occurs when part of the stomach pushes upward through the diaphragm, a large muscle that separates the chest and abdomen. The diaphragm has a small opening called the hiatus through which the esophagus passes before connecting to the stomach. When the stomach pushes through this opening, it forms a hernia, which can lead to various symptoms, including acid reflux, heartburn, and discomfort. While many people with a hiatus hernia may not experience symptoms, others may suffer from chronic digestive issues.
What are the Causes of a Hiatus Hernia?
While the exact cause isn’t always known, several factors can contribute:
(1) Age-Related Weakness
With age, especially after 50, the diaphragm muscles—particularly around the esophageal opening—can weaken, making it easier for the stomach to push upward into the chest.
(2) Increased Abdominal Pressure
Conditions that raise abdominal pressure can contribute, such as:
Obesity
Pregnancy
Chronic coughing (e.g., from smoking or COPD)
- Straining during bowel movements or vomiting
(3) Genetic Factors
A family history may increase risk due to inherited traits like a larger hiatus or weaker connective tissue.
(4) Trauma to the Diaphragm
Injuries from accidents, falls, or surgery can weaken the diaphragm and lead to herniation.
(5) Lifestyle Factors
Smoking, heavy lifting, poor posture, and frequent bending can increase intra-abdominal pressure and strain the diaphragm, raising the risk of hernia.
What are the Symptoms of Hiatus Hernia?
The symptoms of a hiatus hernia can vary depending on the type and severity of the hernia. Many people with a hiatus hernia may not experience noticeable symptoms. However, when symptoms do occur, they can include:
- Heartburn: A burning sensation in the chest or throat, which is often worse after eating or when lying down.
- Acid Reflux: A sour or bitter taste in the mouth caused by stomach acid traveling up the esophagus.
- Chest Pain: This can sometimes mimic the pain of a heart attack and may be aggravated by eating or lying down.
- Difficulty Swallowing (Dysphagia): A sensation of food being stuck in the throat or chest, particularly with larger meals.
- Regurgitation: A sensation of stomach contents, including food or acid, rising up into the mouth.
- Bloating and Fullness: A feeling of bloating or fullness after eating, even after consuming small amounts of food.
- Nausea and Vomiting: In severe cases, especially with paraesophageal hiatus hernia, there may be episodes of nausea and vomiting.
What are the Risk Factors for Hiatus Hernia?
Several factors can increase the risk of developing a hiatus hernia:
- Age: The risk increases with age, especially after the age of 50, due to the weakening of the diaphragm muscles.
- Obesity: Excess abdominal fat puts pressure on the stomach and diaphragm, increasing the risk of a hiatus hernia.
- Pregnancy: The growing uterus can put pressure on the stomach, contributing to the development of a hiatus hernia, especially later in pregnancy.
- Chronic Coughing: Conditions like chronic bronchitis or asthma that lead to prolonged coughing can increase pressure on the abdominal area, making a hiatus hernia more likely.
- Heavy Lifting: Lifting heavy objects repeatedly can strain the diaphragm and abdominal muscles, leading to a higher risk of developing a hernia.
- Genetics: A family history of hiatus hernia may increase the likelihood of developing the condition.
What are the Complications of Hiatus Hernia?
While a hiatus hernia can often be managed without serious complications, untreated or severe cases may lead to more serious issues, including:
- GERD (Gastroesophageal Reflux Disease): A common complication of hiatus hernia, where stomach acid frequently flows back into the esophagus, causing irritation and inflammation.
- Esophagitis: Inflammation of the esophagus due to repeated acid exposure, which can lead to pain, difficulty swallowing, and potential scarring.
- Strangulated Hiatus Hernia: In severe cases of paraesophageal hernia, the blood supply to the part of the stomach that has pushed through the diaphragm can become compromised, leading to a medical emergency.
- Anemia: Chronic bleeding from the esophagus or stomach due to reflux can lead to anemia (low blood levels).
- Esophageal Ulcers: Repeated acid reflux can lead to open sores or ulcers in the esophagus, which may result in bleeding or difficulty swallowing.
- Pulmonary Aspiration: Acid or food particles may be inhaled into the lungs, increasing the risk of aspiration pneumonia, particularly in people with GERD.
Diagnosis of Hiatus Hernia
To diagnose a hiatus hernia, a doctor will typically perform a physical examination, review the patient’s medical history, and may order one or more of the following tests:
(1) Upper Endoscopy (Gastroscopy)
This procedure uses a thin, flexible tube with a small camera at the tip. The tube is gently passed through the mouth and down into the esophagus and stomach. It allows doctors to see the inside of the upper digestive system in real time on a screen. It is usually done under mild sedation to keep the patient comfortable.
(2) Barium Swallow X-ray (Upper GI Series)
In this test, the patient drinks a liquid that contains barium, a substance that coats the inside lining of the esophagus and stomach. After drinking it, a series of X-rays are taken. The barium makes the shape and motion of the digestive tract visible on the X-ray images, allowing doctors to watch how food and liquid move down the esophagus.
(3) Esophageal pH Monitoring
This test tracks the level of acid in the esophagus over a 24-hour period. A thin tube with a sensor is placed through the nose into the esophagus, or a small wireless capsule may be attached to the esophagus during a short endoscopy. The sensor records acid levels and sends the data to a monitor worn by the patient. This helps track when and how often stomach acid flows into the esophagus.
(4) Esophageal Manometry
A test used to measure how well the muscles of the esophagus are working. A thin tube with pressure sensors is inserted through the nose into the esophagus. The patient is asked to swallow several times, and the sensors record how the muscles contract and move food down. It also measures how well the lower esophageal sphincter opens and closes.
Treatment for Hiatus Hernia
Treatment for hiatus hernia typically involves lifestyle modifications, medications, and, in some cases, surgery, depending on the severity of symptoms and complications:
Lifestyle Modifications
- Dietary Changes: Avoiding foods that trigger acid reflux, such as spicy foods, caffeine, chocolate, and fatty foods. Eating smaller meals and not lying down immediately after eating can help reduce symptoms.
- Weight Loss: If overweight, losing weight can reduce abdominal pressure and improve symptoms.
- Elevating the Head of the Bed: Sleeping with the head elevated can help prevent acid reflux and improve symptoms at night.
- Avoiding Tight Clothing: Wearing loose-fitting clothes can reduce pressure on the abdomen and lower esophagus.
Medications
- Antacids: Over-the-counter medications that neutralize stomach acid and provide relief from heartburn and reflux.
- H2-Receptor Antagonists: Drugs that reduce the amount of acid produced by the stomach.
- Proton Pump Inhibitors (PPIs): Stronger medications that block acid production and promote healing of the esophagus.
- Prokinetic Medications: These drugs help improve the movement of food through the digestive system and reduce acid reflux.
Surgical Options
- Fundoplication: A procedure in which the top of the stomach is wrapped around the lower esophagus to prevent acid reflux. This is often recommended for severe cases of GERD or when medications do not provide relief.
- Hiatal Hernia Repair Surgery: In cases of paraesophageal hernia or severe symptoms, surgery may be needed to return the stomach to its proper position and repair the hiatus.
- LINX Device: A magnetic device placed around the lower esophagus to strengthen the LES and prevent acid reflux.
Why Choose Us?
Contact Us

