Get Care
Acute Pancreatitis
What is Acute Pancreatitis?
Acute Pancreatitis is a sudden inflammation of the pancreas, an organ located behind the stomach that plays a crucial role in digestion and blood sugar regulation. The pancreas produces enzymes necessary for digesting food, and when it becomes inflamed, these enzymes begin to attack the pancreas itself, leading to pain, tissue damage, and potential complications. Acute pancreatitis can range from mild discomfort to a life-threatening condition, requiring immediate medical care.
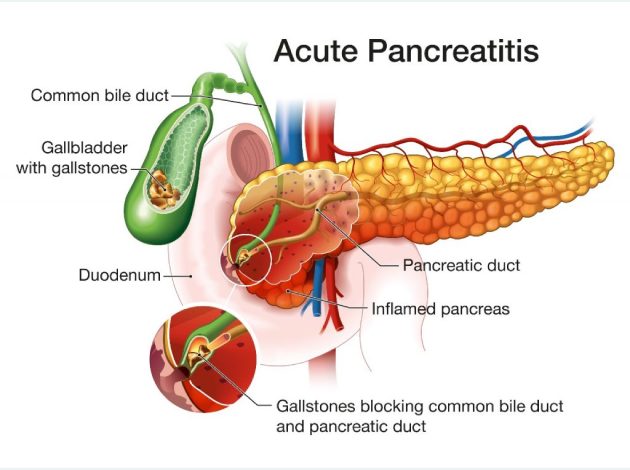
What Causes Acute Pancreatitis?
Acute pancreatitis can be caused by a variety of factors, with some individuals at higher risk due to lifestyle, genetic factors, or existing medical conditions. The most common causes include:
- Gallstones:
Gallstones can block the bile duct, causing a backup of bile into the pancreas, leading to inflammation. This is one of the most common causes of acute pancreatitis. - Alcohol Abuse:
Excessive alcohol consumption is another leading cause of acute pancreatitis. Chronic heavy drinking can irritate the pancreas and lead to inflammation. Even a single episode of heavy drinking can sometimes trigger acute pancreatitis. - High Blood Lipids (Hyperlipidemia):
Elevated levels of fat (triglycerides) in the blood can increase the risk of developing acute pancreatitis. This condition is often associated with metabolic syndromes, diabetes, and obesity. - Medications:
Certain medications, including corticosteroids, diuretics, and certain chemotherapy drugs, can trigger pancreatitis as a side effect. - Abdominal Trauma or Surgery:
Injuries to the pancreas, whether from accidents, falls, or abdominal surgery, can lead to pancreatitis. This may also include complications from gallbladder removal surgery. - Infections:
Viral infections like mumps, coxsackievirus, and HIV can sometimes lead to acute pancreatitis. Bacterial infections, particularly those affecting the gallbladder, can also increase the risk. - Genetic Factors:
Certain genetic conditions or inherited disorders, such as cystic fibrosis or hereditary pancreatitis, can predispose individuals to acute pancreatitis. - Pancreatic Duct Obstruction
Obstruction of the pancreatic duct due to tumors or cysts can disrupt the normal function of the pancreas, leading to inflammation.
What Are the Symptoms of Acute Pancreatitis?
The symptoms of acute pancreatitis can vary in severity, but common signs include:
- Severe Abdominal Pain:
The hallmark symptom of acute pancreatitis is sudden, severe pain in the upper abdomen, which may radiate to the back. The pain can be intense and worsen after eating, especially fatty foods. - Nausea and Vomiting:
Many individuals with acute pancreatitis experience nausea and vomiting, often as a result of the abdominal pain and digestive issues. - Fever:
Infection or inflammation of the pancreas can cause a low-grade fever. A high fever may indicate a more severe infection or complications. - Rapid Heart Rate and Low Blood Pressure:
Inflammation and the body’s response to pain and infection can lead to an elevated heart rate (tachycardia) and low blood pressure (hypotension). - Swollen or Tender Abdomen:
The abdomen may appear distended or swollen due to inflammation. Touching or pressing on the abdomen can cause significant discomfort. - Jaundice:
If the inflammation affects the bile ducts or causes blockages, jaundice (yellowing of the skin and eyes) may develop, indicating a problem with bile flow. - Indigestion:
In some cases, individuals with acute pancreatitis may have difficulty digesting food, leading to bloating, indigestion, or a loss of appetite.
How is Acute Pancreatitis Diagnosed?
Diagnosing acute pancreatitis involves a combination of physical examination, medical history, and diagnostic tests to confirm the inflammation and assess its severity. Key diagnostic methods include:
- Blood Tests:
Blood tests are crucial in diagnosing acute pancreatitis. Elevated levels of pancreatic enzymes, such as amylase and lipase, are often indicative of pancreatitis. Liver enzymes and other markers may also be tested to assess the impact on liver function. - Abdominal Ultrasound:
An abdominal ultrasound uses sound waves to create images of the pancreas, gallbladder, and surrounding organs. It is particularly useful in detecting gallstones, which are a common cause of acute pancreatitis. - CT Scan (Computed Tomography):
A CT scan provides detailed images of the pancreas and surrounding structures, allowing doctors to evaluate the severity of inflammation, identify complications (such as cysts or abscesses), and rule out other conditions. - MRI (Magnetic Resonance Imaging):
MRI may be used for a more detailed view of the pancreas and bile ducts, especially in cases where a CT scan is inconclusive. It can also help identify complications like pancreatic pseudocysts or necrosis. - Endoscopic Ultrasound (EUS):
In some cases, an EUS may be performed, where a small camera is inserted into the digestive tract to get closer views of the pancreas and bile ducts. It is especially helpful for detecting gallstones and other blockages. - Endoscopic Retrograde Cholangiopancreatography (ERCP):
If the cause of pancreatitis is believed to be a bile duct obstruction (e.g., gallstones), ERCP can be used both for diagnosis and treatment. This procedure allows the doctor to visualize the bile ducts and remove any blockages.
How is Acute Pancreatitis Treated?
Treatment for acute pancreatitis aims to reduce inflammation, manage pain, and prevent complications. The approach can vary depending on the severity of the condition and the underlying cause:
- Hospitalization and Observation:
In most cases, acute pancreatitis requires hospitalization for close monitoring and management of symptoms. Patients are typically observed for signs of complications, such as infection or organ failure. - Fasting and Nutritional Support:
To allow the pancreas to rest and heal, patients are often advised to refrain from eating or drinking for a period of time. Once the acute phase has passed, nutrition may be introduced gradually, typically through intravenous (IV) fluids or a feeding tube. - Pain Management:
Pain relief is an essential part of treatment. Pain medications, including narcotics and non-steroidal anti-inflammatory drugs (NSAIDs), are used to manage the intense abdominal pain that typically accompanies acute pancreatitis. - Intravenous Fluids (IV):
Dehydration is common in acute pancreatitis, and IV fluids are administered to maintain hydration, restore electrolyte balance, and support organ function. - Treating the Underlying Cause:
If gallstones are the cause of the pancreatitis, they may be removed surgically. If alcohol abuse is the contributing factor, patients are advised to stop drinking and may receive counseling for alcohol dependence. For other causes, specific treatments (such as stopping medications or addressing hyperlipidemia) may be required. - Antibiotics:
If there is a suspected or confirmed infection of the pancreas (pancreatic abscess or infected pancreatic necrosis), antibiotics may be prescribed to treat the infection. - Surgery:
In severe cases, surgery may be required to remove damaged tissue, drain abscesses, or remove gallstones. If the pancreas has suffered significant damage, surgery may be necessary to treat complications like pseudocysts or pancreatic necrosis.
What Are the Complications of Acute Pancreatitis?
While many cases of acute pancreatitis resolve with treatment, there are potential complications that may arise, especially in severe cases:
- Pancreatic Necrosis:
This occurs when the pancreas tissue dies due to prolonged inflammation. Necrosis can lead to infection, which is life-threatening and may require surgical intervention. - Pseudocysts:
Pancreatic pseudocysts are fluid-filled sacs that can form in or around the pancreas after an episode of pancreatitis. These pseudocysts can cause pain, infection, or rupture, which requires medical treatment. - Infection:
Infected pancreatic tissue or abscesses can develop in severe cases. Infections may spread to other organs and are often treated with antibiotics or surgery. - Organ Failure:
In rare cases, acute pancreatitis can cause failure of vital organs like the kidneys, lungs, or heart. Organ failure can be life-threatening and requires intensive medical care. - Chronic Pancreatitis:
Repeated episodes of acute pancreatitis can lead to permanent damage to the pancreas, resulting in chronic pancreatitis, which affects its ability to produce digestive enzymes and insulin.
Why Choose Us?
Contact Us

