Get Care
Diverticulitis
What is Diverticulitis?
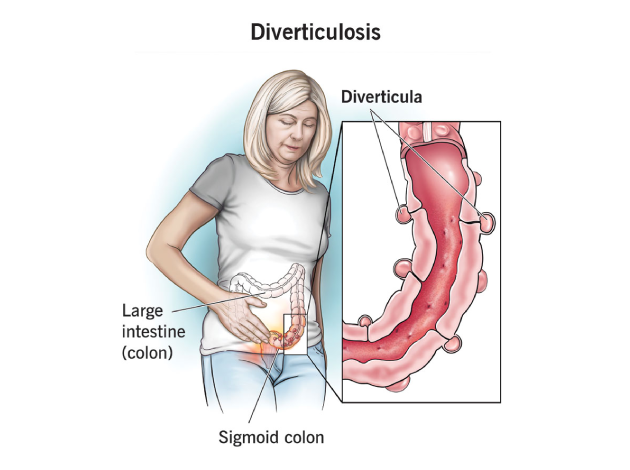
Diverticulitis is a condition that occurs when small, bulging pouches (called diverticula) in the wall of the colon become inflamed or infected. These pouches form as a result of weak spots in the colon’s lining, where the pressure from stool causes the intestinal wall to bulge out, creating pockets. While diverticulosis refers to the presence of these pouches without symptoms, diverticulitis occurs when these pouches become irritated or infected, leading to more serious complications.
Diverticulitis is more common in individuals over the age of 40 and is often linked to a low-fiber diet, which can cause constipation and increased pressure in the colon. However, it can also occur in people with no apparent risk factors.
what are the causes of diverticulitis?
Diverticulitis occurs when small pouches (diverticula) that form in the wall of the colon become inflamed or infected. While the exact cause is not always clear, several factors are believed to contribute:
(1) Blocked Diverticula
Trapped stool or food particles can block the opening of a diverticulum, leading to bacterial overgrowth, inflammation, or infection.
(2) Low-Fiber Diet
A diet low in fiber leads to hard stools and increased pressure in the colon, which can promote the formation of diverticula and their subsequent inflammation.
(3) Chronic Constipation
Straining during bowel movements raises pressure in the colon, making it easier for diverticula to form and become inflamed.
(4) Age
The risk of diverticulitis increases with age, as the colon wall weakens over time.
(5) Obesity and Sedentary Lifestyle
Being overweight and physically inactive are associated with a higher risk of developing diverticulitis.
(6) Smoking
Smoking has been linked to an increased risk of complications and recurrence of diverticulitis.
(7) Certain Medications
Use of NSAIDs (e.g., ibuprofen), steroids, or opioids may increase the risk of diverticulitis or worsen existing inflammation.
Symptoms of Diverticulitis
Diverticulitis often presents with a range of gastrointestinal and systemic symptoms, which can vary in severity depending on the extent of inflammation or infection,it Includes:
Abdominal Pain: The most common and noticeable symptom is persistent pain, usually in the lower left side of the abdomen. The pain may start as mild but can become sharp and more intense over time. It often worsens with movement or after meals.
Fever and Chills: These are signs that infection is present. As the body’s immune system responds to the inflamed or infected diverticula, it raises the body temperature, leading to fever, often accompanied by chills or shivering.
Nausea and Vomiting: Inflammation of the colon can irritate surrounding tissues or slow down bowel function, leading to nausea. In more severe cases or if a blockage occurs, this can progress to vomiting.
Changes in Bowel Habits: Many patients experience constipation, although diarrhea may also occur in some cases. These changes result from inflammation affecting normal bowel movements and motility.
Bloating and Gas: Patients may feel a sense of fullness, pressure, or distention in the abdomen due to trapped gas and inflammation, which can be uncomfortable and persistent.
Abdominal Tenderness: The affected area, often the lower left abdomen, becomes sensitive or painful to touch, especially during physical examination by a healthcare provider.
Loss of Appetite: Inflammation and abdominal discomfort can reduce hunger, leading to a noticeable decrease in appetite and sometimes unintended weight loss.
Urinary Symptoms: In some cases, especially when the inflamed area is near the bladder, patients may experience frequent urination, urgency, or discomfort during urination due to irritation or pressure on the urinary tract.
What are the Risk factors of Diverticulitis?
Several factors can increase the risk of developing diverticulitis:
- Aging
– Risk increases after age 40 due to weakening of the colon wall. - Low-Fiber Diet
– Diets low in fiber can cause constipation and increase pressure in the colon. - Lack of Physical Activity
– Sedentary lifestyle is linked to higher risk. - Obesity
– Especially abdominal (central) obesity increases the chance of inflammation. - Smoking
– Associated with a greater risk and more severe disease. - Certain Medications
– Long-term use of NSAIDs, steroids, or opioids can increase risk. - History of Diverticulosis
– Having diverticula (diverticulosis) is a direct precursor to diverticulitis.
What are the Complications of Diverticulitis?
If not treated properly, diverticulitis can lead to several serious complications:
Abscess
– A pocket of pus may form around the inflamed diverticula, causing pain, fever, and swelling.Perforation
– A tear or hole in the colon wall can result in peritonitis, a life-threatening abdominal infection.Bowel Obstruction
– Scar tissue or swelling from repeated inflammation may partially or completely block the colon.Fistula
– An abnormal connection may form between the colon and other organs (like the bladder or skin), often requiring surgery.Bleeding
– Though rare, diverticulitis can cause rectal bleeding.Chronic Symptoms
– Some people may experience ongoing abdominal pain or bowel changes even after treatment.
Diagnosis of Diverticulitis
Diverticulitis is diagnosed through medical history, physical exam, lab tests, and imaging. It occurs when small pouches in the colon (diverticula) become inflamed or infected. Early diagnosis is important to distinguish it from other abdominal conditions like appendicitis or colorectal cancer.
(1) Clinical History and Presentation
The diagnostic process begins with a thorough review of the patient’s symptoms and medical history. Most patients with diverticulitis report sudden onset abdominal pain, typically localized in the lower left quadrant of the abdomen. This pain may be constant and worsen over time. Accompanying symptoms may include fever, chills, nausea, vomiting, and changes in bowel habits, such as constipation or diarrhea. Some patients may also report bloating or urinary symptoms, especially if the inflamed diverticula are near the bladder. A history of diverticulosis, previous similar episodes, or a low-fiber diet can raise clinical suspicion.
(2) Physical Examination
On physical examination, a physician will palpate the abdomen to assess tenderness. In cases of diverticulitis, there is typically marked tenderness in the lower left quadrant. If the inflammation has progressed to involve the peritoneum (peritonitis), signs such as muscle guarding, rigidity, and rebound tenderness may be present. The presence of these signs can indicate complications such as abscess formation or perforation. A digital rectal examination may be performed to check for rectal masses or bleeding.
(3) Laboratory Tests
Laboratory testing supports the clinical diagnosis by identifying signs of inflammation or infection:
- A complete blood count (CBC) often shows an elevated white blood cell (WBC) count, reflecting systemic infection or localized inflammation.
- C-reactive protein (CRP), an acute-phase reactant, is frequently elevated in diverticulitis and may correlate with disease severity.
- Electrolyte levels are evaluated to check for dehydration or systemic response.
- Liver function tests and pancreatic enzymes (amylase/lipase) may also be performed to rule out other abdominal pathologies like hepatitis or pancreatitis that can mimic diverticulitis.
(4) Imaging Studies
Imaging is the cornerstone of diagnosis, especially when clinical symptoms are unclear or complications are suspected.
(5) CT Scan (Computed Tomography)
A contrast-enhanced CT scan of the abdomen and pelvis is the most accurate and widely used imaging modality for diagnosing diverticulitis. It helps confirm the diagnosis by showing:
- Colonic wall thickening
- Pericolonic fat stranding (a hallmark sign of inflammation)
- Presence of diverticula
- Detection of complications such as abscesses, perforation, fistulas, or bowel obstruction
- CT imaging is also used to classify the severity of the disease (uncomplicated vs. complicated), which directly influences treatment decisions.
- Ultrasound
- While less commonly used, abdominal ultrasound may be employed in certain populations—such as pregnant women or where CT is unavailable. Ultrasound can detect localized inflammation and abscess formation but is generally less sensitive than CT.
(6) Colonoscopy (After Acute Phase)
Colonoscopy is avoided during the acute phase of diverticulitis due to the risk of bowel perforation. However, once symptoms have resolved—usually after 6 to 8 weeks—a colonoscopy is recommended to:
Confirm the presence of diverticulosis
Exclude colorectal cancer
Identify polyps or other abnormalities
This follow-up procedure is especially important in patients with first-time diverticulitis or in those over the age of 50.
Treatment of Diverticulitis
The treatment for diverticulitis depends on the severity of the condition. Mild cases can often be managed at home, while more severe cases may require hospitalisation and invasive treatments. Treatment options include:
(1) Dietary Modifications:
- Clear Liquid Diet: For mild cases, a clear liquid diet may be recommended to rest the digestive system and reduce inflammation.
- Gradual Introduction of Solid Foods: Once symptoms improve, solid foods, especially high-fiber foods, will be gradually reintroduced to help prevent future flare-ups.
- Fiber Supplements: Fiber helps soften stools and ease bowel movements, reducing strain on the colon.
(2) Antibiotics:
If there is an infection, antibiotics are often prescribed to treat the infection and reduce inflammation. These can be given orally for mild cases, or intravenously in more severe cases.
(3) Pain Management:
Over-the-counter pain relievers, such as acetaminophen, may be used to relieve discomfort. However, nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen should be avoided as they may increase the risk of bleeding and complications.
(4) Hospitalisation:
If symptoms are severe, such as high fever, intense pain, or vomiting, hospitalisation may be required. Intravenous antibiotics, fluids, and more aggressive pain management may be necessary.
(5) Surgery:
In severe cases, surgery may be required. Surgical options include:
- Bowel Resection: Removal of the affected portion of the colon may be necessary if there is significant damage, or if there are complications like perforation, abscess, or persistent bleeding.
- Colostomy: In some cases, a temporary or permanent colostomy may be performed, where the colon is diverted to an opening in the abdominal wall for waste to be collected in a bag.
(6) Lifestyle Changes:
- Increased Fiber Intake: Once the acute phase of diverticulitis has resolved, a high-fiber diet is recommended to promote healthy bowel movements and prevent further flare-ups. Fiber-rich foods include fruits, vegetables, whole grains, and legumes.
- Regular Exercise: Exercise promotes bowel function and can help reduce the risk of constipation, which is a contributing factor to diverticulitis.
- Hydration: Drinking plenty of fluids helps prevent constipation and aids in digestion.
Why Choose Us?
Contact Us

