Get Care
Incisional Hernia
What is an Incisional Hernia?
An incisional hernia occurs when tissue or an organ, typically part of the intestine, protrudes through a weak spot in the abdominal wall at the site of a previous surgical incision. This type of hernia is a common complication after abdominal surgery and can develop weeks, months, or even years after the procedure. The area where the surgical incision was made forms a natural weak point in the abdominal wall, which can become vulnerable to herniation, especially if the healing process was compromised or the abdominal pressure increased.Incisional hernias are most commonly found in patients who have undergone major abdominal surgeries such as those for appendectomy, C-section, hernia repair, or colorectal procedures. Factors such as infection, poor wound healing, or increased intra-abdominal pressure can contribute to the development of an incisional hernia.
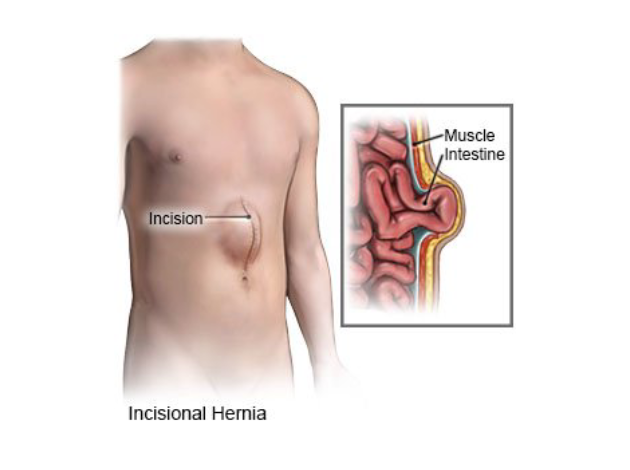
What Causes an Incisional Hernia?
The primary cause of an incisional hernia is a previous abdominal surgery. Several factors can lead to the formation of a hernia at the site of a surgical incision:
- Surgical Site Weakness: Surgical incisions create a gap in the abdominal wall, which may not heal completely or may heal in a weakened state, allowing tissue to protrude through.
- Increased Abdominal Pressure: Activities that increase intra-abdominal pressure, such as heavy lifting, chronic coughing, obesity, constipation, or pregnancy, can exacerbate the weakness in the abdominal wall, leading to herniation.
- Poor Healing: Infections, improper wound care, or poor nutrition during recovery can impair the healing process, leading to the formation of scar tissue that is not as strong as the surrounding healthy tissue.
- Obesity or Weight Gain: Excess weight can place additional pressure on the abdominal wall and contribute to the development of an incisional hernia.
- Age: Older adults are at a higher risk due to natural weakening of tissues and slower healing processes.
- Pre-existing Medical Conditions: Conditions such as diabetes, smoking, or immunocompromised states can increase the likelihood of poor wound healing and contribute to hernia formation.
What are the Signs and Symptoms of an Incisional Hernia?
The signs and symptoms of an incisional hernia can vary depending on its size and location, but common symptoms include:
- Visible Bulge or Lump: A soft, protruding bulge near the site of a previous surgical incision is the hallmark sign of an incisional hernia. This bulge may be more noticeable when coughing, straining, or standing, and may reduce or disappear when lying down.
- Pain or Tenderness: The area around the hernia may be painful, particularly when moving, lifting, or coughing. The pain is usually mild but can be more severe in larger or complicated hernias.
- Discomfort During Physical Activity: Activities that increase abdominal pressure, such as lifting heavy objects, bending, or intense physical exertion, may trigger discomfort or pain at the site of the hernia.
- Bowel Obstruction: In severe cases, part of the intestine may become trapped in the hernia, leading to symptoms like nausea, vomiting, and an inability to pass stool or gas. This is a medical emergency and requires prompt treatment.
What are the Risk Factors for Incisional Hernia?
Several factors can increase the likelihood of developing an incisional hernia after surgery:
- Previous Abdominal Surgery: Any prior abdominal surgery, particularly if the incision was large or involved a complicated healing process, increases the risk of developing an incisional hernia.
- Obesity: Overweight individuals are more likely to experience increased intra-abdominal pressure, which can weaken the surgical site and lead to hernia formation.
- Poor Wound Healing: Conditions such as diabetes, smoking, or infections at the surgical site can impair the healing process, contributing to the formation of a hernia.
- Age: Older adults have a higher risk due to natural tissue weakening and slower healing processes.
- Increased Intra-Abdominal Pressure: Conditions like chronic coughing, heavy lifting, or constipation can place additional strain on the abdominal wall.
- Multiple Surgeries: Patients who have undergone several abdominal surgeries may have weaker abdominal walls and a higher chance of developing hernias.
- Immunocompromised States: Individuals with weakened immune systems or those on immunosuppressive medications are more likely to develop complications after surgery, including hernias.
What are the Complications of an Incisional Hernia?
If left untreated or if complications arise, incisional hernias can lead to serious conditions, including:
- Incarceration: When part of the intestine or other tissue becomes trapped in the hernia sac, it cannot be pushed back into the abdomen. This can cause pain, swelling, and discomfort.
- Strangulation: A more serious complication, strangulation occurs when the blood supply to the trapped tissue is cut off, leading to tissue death (gangrene). This is a medical emergency and requires immediate surgery.
- Bowel Obstruction: If the intestine becomes trapped in the hernia, it can lead to a blockage in the digestive tract, causing severe pain, nausea, vomiting, and the inability to pass stool or gas.
- Recurrent Hernia: Even after surgical repair, there is a risk of the hernia recurring, especially if the underlying cause (such as obesity or improper healing) is not addressed.
Diagnosis of Incisional Hernia
An incisional hernia develops at the site of a previous surgical incision where the abdominal wall has not healed properly, resulting in a weakness that allows internal tissues or organs to protrude. Accurate diagnosis is essential for proper treatment planning, especially as these hernias can vary in size and complexity.
(1) Physical Examination (Primary Diagnostic Tool)
The first and most important step in diagnosing an incisional hernia is a thorough clinical assessment by a healthcare provider.
During the Examination:
- The patient is usually asked to stand upright and strain or cough, which increases intra-abdominal pressure and may make the hernia more prominent.
- The doctor inspects the surgical scar or incision site for a visible bulge or swelling that becomes more obvious during physical exertion.
- Palpation (gently pressing on the area) is performed to assess:
- Size and shape of the hernia
- Reducibility (whether it can be pushed back into the abdomen)
- Tenderness or firmness, which could indicate incarceration (trapped tissue) or strangulation (compromised blood flow)
- The presence of a hernia sac, especially in cases with recurrent symptoms
In cases of large or easily visible hernias, this step alone may be enough to confirm the diagnosis.
(2) Ultrasound Imaging
Ultrasound is often the first-line imaging tool when the physical exam is inconclusive or when a smaller or hidden hernia is suspected.
- Non-invasive and painless, this test uses sound waves to produce images of soft tissues.
- It helps confirm the presence, size, and contents of the hernia sac.
- Particularly useful in:
- Obese patients where physical examination is difficult
- Early-stage hernias or small fascial defects
- Identifying complications such as bowel entrapment or fluid collections
(3) CT Scan (Computed Tomography)
CT scanning is considered the gold standard for evaluating complex, recurrent, or large incisional hernias.
- Provides detailed cross-sectional images of the abdominal wall, hernia contents, and their relationship to surrounding organs.
- Essential for surgical planning, especially if:
- The hernia is not fully reducible
- There are multiple defects
- Internal organs such as bowel or omentum are involved
- Also used to detect signs of obstruction, inflammation, or strangulation.
CT is particularly valuable in cases where hernias are not clearly visible externally or when the patient presents with abdominal pain or complications.
(4) MRI (Magnetic Resonance Imaging)
While not commonly required, MRI may be used in special cases, especially when:
- There is a need for high-resolution soft tissue detail
- CT findings are inconclusive
- The patient cannot undergo CT due to contrast allergy or radiation sensitivity
- Evaluation is needed for recurrent hernias, especially when previous mesh repairs complicate imaging
MRI can clearly outline the muscular layers, fascial defects, and any trapped or ischemic tissues, helping differentiate a true hernia from other masses or postoperative fluid collections.
Treatment of Incisional Hernia
The treatment of an incisional hernia generally involves surgical repair. The two main options for surgery are:
(1) Open Surgery (Herniorrhaphy): In this traditional approach, the surgeon makes an incision over the hernia site, pushes the herniated tissue back into place, and repairs the abdominal wall with sutures. A mesh may be used to strengthen the weakened area.
(2) Laparoscopic Surgery: This minimally invasive procedure involves smaller incisions, through which a camera and instruments are inserted to repair the hernia. Laparoscopic surgery typically results in less pain, quicker recovery, and fewer complications compared to open surgery.
In cases of incarcerated or strangulated hernias, emergency surgery may be required to relieve the obstruction and repair the hernia.
Lifestyle and Supportive Measures
To help manage and reduce the risk of complications, the following lifestyle measures are recommended:
- Maintain a Healthy Weight: Losing excess weight can reduce the strain on the abdominal wall and help prevent the recurrence of the hernia.
- Avoid Straining: Avoid heavy lifting, straining during bowel movements, or any activity that increases intra-abdominal pressure.
- Manage Chronic Cough: If you have chronic coughing (e.g., from smoking, asthma, or respiratory conditions), seek treatment to alleviate the coughing, which can exacerbate the hernia.
- Postoperative Care: After surgery, it is important to follow the doctor’s instructions regarding rest, activity restrictions, and wound care to promote healing and reduce the risk of recurrence.
- Strengthen Core Muscles: Core exercises, once cleared by a healthcare provider, can help strengthen the abdominal muscles and prevent further weakening.
Prognosis
With proper treatment, most incisional hernias can be successfully repaired with minimal complications. Surgical intervention is highly effective in the majority of cases, with most patients returning to normal activities within a few weeks. The risk of recurrence is generally low, especially when the underlying causes, such as obesity or poor healing, are addressed.
Why Choose Us?
Contact Us

