Get Care
Hydrocele
What is Hydrocele?
A hydrocele is a condition characterized by the accumulation of fluid within the sac surrounding the testicle, resulting in swelling in the scrotum. The sac, called the tunica vaginalis, normally contains a small amount of fluid to lubricate the testicle and allow it to move freely. However, when excess fluid accumulates, it leads to the formation of a hydrocele. Hydroceles are typically painless and are often discovered during a routine physical exam.While hydroceles can occur at any age, they are most common in newborns and older men. In newborns, a hydrocele often resolves on its own within the first year of life. In adults, it may develop due to injury, inflammation, or infection in the scrotum. Hydroceles can occur on one or both sides of the scrotum.
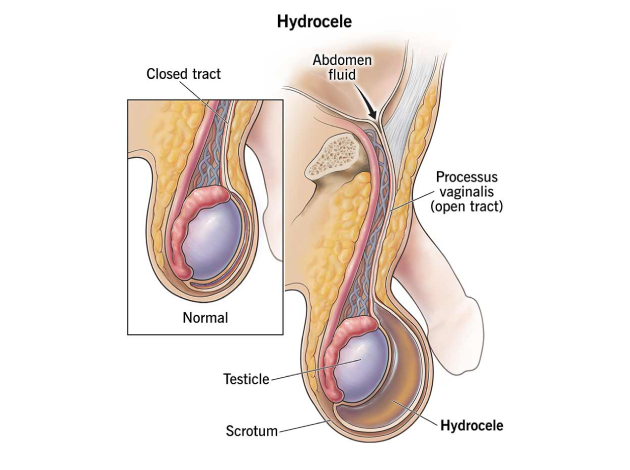
What Causes Hydrocele?
Hydroceles can be classified into two main types: communicating and non-communicating, based on the underlying cause.
(1) Communicating Hydrocele:
- This type occurs when the processus vaginalis, a canal that is normally present during fetal development, fails to close after birth. This allows fluid from the abdominal cavity to flow into the scrotum, causing swelling. Communicating hydroceles are often found in newborns and are more likely to resolve on their own.
- In adults, a communicating hydrocele may be associated with a hernia, where a portion of the intestine or abdominal tissue protrudes into the scrotum along with the fluid.
(2) Non-Communicating Hydrocele:
- This type occurs when fluid accumulates in the tunica vaginalis without any communication with the abdominal cavity. The cause of this type is usually unknown, but it can result from injury, infection, or inflammation of the scrotum.
- Non-communicating hydroceles are more commonly seen in adult men and are typically not associated with other conditions.
What are the Signs and Symptoms of Hydrocele?
The primary symptom of a hydrocele is the swelling of the scrotum, which may vary in size depending on the amount of fluid accumulated. The swelling is usually painless, but in some cases, it can cause discomfort due to the increased size of the scrotum. Specific symptoms include:
- Painless Scrotal Swelling: The swelling may be soft, smooth, and translucent, and it may fluctuate in size, becoming more noticeable during the day or after periods of activity.
- Fullness in the Scrotum: A feeling of heaviness or fullness in the scrotum can occur, especially when standing for extended periods.
- Increased Size of the Scrotum: The scrotum may become visibly enlarged, which can be noticeable when compared to the unaffected side.
- No Pain or Tenderness: Hydroceles are typically painless, although they may cause some discomfort due to their size, particularly when walking or standing.
In more severe cases or when complications arise, additional symptoms may include:
- Discomfort or Pain: Rarely, hydroceles can become large enough to cause pressure or pain in the scrotum.
- Infection or Inflammation: In cases where a hydrocele is caused by infection or injury, symptoms such as redness, warmth, and tenderness may develop.
What are the Risk Factors for Hydrocele?
While many hydroceles develop without any obvious risk factors, certain conditions can increase the likelihood of developing a hydrocele, including:
- Age: Hydroceles are more common in newborns, but they also occur in older men, particularly those over the age of 40.
- Infection or Inflammation: Conditions like epididymitis (inflammation of the epididymis), orchitis (testicular infection), or a previous infection in the scrotum can increase the risk of hydrocele formation.
- Trauma or Injury: Scrotal trauma, surgery, or injury to the testicles or scrotum can lead to the development of a hydrocele.
- Hernias: In some cases, a hydrocele may be associated with a hernia, especially in communicating hydroceles where there is a direct communication between the scrotum and the abdomen.
- Previous Abdominal Surgery: Men who have undergone abdominal or groin surgeries may be at increased risk for hydroceles.
What are the Complications of Hydrocele?
In most cases, a hydrocele is a benign condition that does not lead to serious complications. However, complications can arise in certain situations:
- Infection: If the hydrocele is associated with an infection in the scrotum, there is a risk of developing an abscess or spreading the infection to other parts of the body.
- Testicular Atrophy: In rare cases, prolonged pressure from a large hydrocele can lead to reduced blood flow to the testicle, which may result in testicular atrophy (shrinkage of the testicle).
- Discomfort or Pain: Large hydroceles can cause discomfort, particularly when walking, standing, or engaging in physical activities.
- Hernia Formation: A communicating hydrocele may be associated with an inguinal hernia, in which a portion of the intestine pushes through the abdominal wall into the scrotum. This can lead to complications such as bowel obstruction or strangulation, which requires immediate medical attention.
Diagnosis of Hydrocele
A hydrocele is a fluid-filled sac surrounding a testicle that causes swelling in the scrotum. It is typically painless and benign, but proper diagnosis is important to distinguish it from other scrotal conditions such as inguinal hernias, testicular tumors, or infections. Most hydroceles can be diagnosed through a clinical examination, though imaging may be necessary in certain cases.
(1) Physical Examination (Initial Step)
The first and most crucial step in diagnosing a hydrocele is a thorough physical examination by a healthcare provider.
What the Doctor Will Look For:
- A smooth, soft, and non-tender swelling on one or both sides of the scrotum.
- The swelling is usually in front of and below the testicle.
- It may vary in size throughout the day but does not typically cause pain.
- Fluctuation in size or discomfort may occur if the hydrocele is large.
The physician will gently palpate the scrotum, feeling for:
- The consistency of the mass (fluid-filled vs solid)
- The position of the testicle in relation to the swelling
- Any signs of tenderness, which might suggest infection or another condition
In infants and young boys, the hydrocele may be associated with a patent processus vaginalis, and the swelling can fluctuate as abdominal fluid moves in and out.
(2) Transillumination Test (Simple & Classic Diagnostic Tool)
The transillumination test is a quick and non-invasive bedside technique often used to confirm the presence of a hydrocele.
How it Works:
- A penlight or flashlight is placed against the back of the scrotum in a dark room.
- If a hydrocele is present, the light passes through the fluid-filled sac, causing the scrotum to glow with a reddish or pink hue.
- This confirms the presence of clear fluid, distinguishing a hydrocele from a solid mass like a tumor or blood-filled swelling (hematocele).
Transillumination is especially helpful in infants and young children, where imaging may not always be necessary if the diagnosis is clear.
(3) Scrotal Ultrasound (Definitive Confirmation Tool)
If the diagnosis is uncertain, if there are atypical features, or if other conditions are suspected, a scrotal ultrasound is the imaging test of choice.
What Ultrasound Evaluates:
- Size and extent of the hydrocele
- Whether the fluid is clear or complex (may suggest infection or bleeding)
- The position and appearance of the testicle
- Presence of associated conditions, such as:
- Testicular torsion
- Tumors or masses
- Inguinal hernia
Ultrasound is safe, painless, and highly accurate, making it the standard imaging method in most adult cases.
(4) CT Scan or MRI (Advanced Imaging – Rarely Needed)
Advanced imaging like CT or MRI is rarely needed for diagnosing a simple hydrocele but may be used in complex or unclear cases, especially when:
- Other scrotal or abdominal conditions (e.g., hernias, lymphadenopathy, tumors) are suspected
- The hydrocele is recurrent, rapidly enlarging, or atypical
- There is a concern about underlying malignancy, particularly in older adults
These imaging techniques provide a more detailed view of the surrounding structures, including the abdominal cavity, inguinal canal, and retroperitoneal space.
Treatment of Hydrocele
The treatment of a hydrocele depends on the severity of the condition, the underlying cause, and the patient’s symptoms. Options include:
- Observation: In many cases, particularly in newborns, hydroceles resolve on their own without the need for medical intervention. Regular follow-up visits may be recommended to monitor the condition.
- Surgical Repair: If the hydrocele is large, persistent, or causing discomfort, surgery may be required. The two primary surgical options are:
- Hydrocelectomy: The surgical removal of the fluid-filled sac. This procedure involves making an incision in the scrotum, removing the hydrocele, and closing the sac to prevent recurrence.
- Laparoscopic Hydrocelectomy: A minimally invasive option where small incisions are made, and a camera is used to guide the surgery. This approach results in smaller scars, less pain, and faster recovery.
- Needle Aspiration: In some cases, a needle may be used to drain the fluid from the hydrocele. However, this method has a high rate of recurrence and is not considered a long-term solution.
- Sclerotherapy: After drainage, a sclerosing agent may be injected into the sac to help prevent the fluid from re-accumulating. This is sometimes used in combination with needle aspiration but is less commonly employed.
Lifestyle and Supportive Measures
For patients with small or uncomplicated hydroceles, the following supportive measures may be recommended:
- Avoiding Heavy Lifting: Strenuous activities and heavy lifting can increase intra-abdominal pressure and may worsen the hydrocele.
- Proper Scrotal Support: Wearing supportive underwear or a scrotal support garment can reduce discomfort and provide relief.
- Regular Monitoring: For smaller hydroceles, regular follow-up appointments with a healthcare provider are essential to monitor for changes in size or symptoms.
Prognosis
With appropriate treatment, the prognosis for hydrocele is excellent. Most cases resolve successfully, either on their own or after surgery. The recurrence rate following surgical intervention is low, especially when performed by an experienced surgeon. Although the condition is generally not serious, it is important to address any underlying causes, such as infection or hernia, to avoid complications.
Why Choose Us?
Contact Us

