Get Care
Abdominal Tuberculosis
What is Abdominal Tuberculosis?
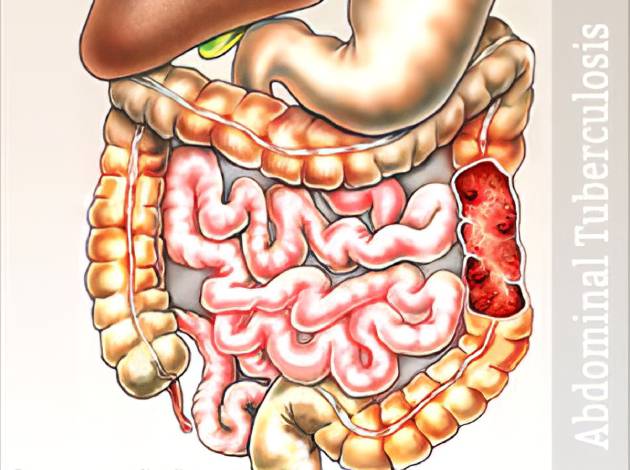
Abdominal Tuberculosis (TB) is a form of extrapulmonary tuberculosis that affects various organs within the abdominal cavity. It can involve the gastrointestinal tract, peritoneum (lining of the abdominal cavity), mesenteric lymph nodes, liver, spleen, and, less commonly, the pancreas. Caused by Mycobacterium tuberculosis, the same bacteria responsible for pulmonary TB, this condition poses diagnostic challenges due to its non-specific symptoms and ability to mimic other abdominal diseases, including Crohn’s disease, malignancies, and appendicitis.
What are the Causes of Abdominal Tuberculosis?
Abdominal TB is caused by Mycobacterium tuberculosis and can spread to the abdomen in the following ways:
Hematogenous Spread
TB from the lungs can enter the bloodstream and infect abdominal organs like lymph nodes, intestines, or peritoneum—especially when the immune system fails to contain it.Ingestion of Infected Sputum
Swallowing TB-infected sputum (common in pulmonary TB) may lead to gastrointestinal infection, especially in the ileocecal region.Contiguous Spread from Nearby Organs
TB from adjacent organs like the spine (Pott’s disease), fallopian tubes, or kidneys can spread directly to abdominal tissues.Reactivation of Latent TB
Latent TB can reactivate in immunocompromised individuals, affecting abdominal organs.
Common Triggers: HIV/AIDS, diabetes, renal failure, immunosuppressive drugs (steroids, chemotherapy), and malnutrition.
What are the Signs and Symptoms of Abdominal Tuberculosis?
Abdominal TB often presents with vague, long-standing symptoms that mimic other GI conditions. Common signs include:
Chronic Abdominal Pain: Typically dull and persistent, usually in the right lower abdomen (ileocecal area).
Unexplained Weight Loss: Gradual, unintended loss due to inflammation, poor appetite, and malabsorption.
Loss of Appetite: Often paired with early satiety and general discomfort.
Low-Grade Evening Fever: Mild fever, more noticeable in the evenings, with sweating.
Abdominal Distension: Feeling of fullness or visible swelling from fluid (ascites) or obstruction.
Altered Bowel Habits: Diarrhea, constipation, or alternating patterns, sometimes with mucus.
Palpable Mass: A firm lump in the lower right abdomen, especially in ileocecal TB.
Ascites: Fluid buildup in the abdomen, often straw-colored and protein-rich.
Night Sweats: Heavy sweating at night, typical in systemic TB.
Fatigue: Ongoing tiredness and weakness due to inflammation and poor nutrition.
In advanced stages, complications like obstruction, perforation, or fistula may develop.
What are the Risk Factors for Abdominal Tuberculosis?
The likelihood of developing abdominal TB increases with:
- Immunocompromised conditions, especially HIV/AIDS
- Malnutrition
- Chronic renal failure
- Diabetes mellitus
- Organ transplantation
- Previous exposure to or treatment for TB
- Poor sanitary conditions and overcrowding
- Use of biologic therapies, especially anti-TNF drugs in autoimmune diseases.
What are the Complications of Abdominal Tuberculosis?
If not diagnosed and treated promptly, abdominal TB can lead to serious complications such as:
- Intestinal obstruction due to stricture formation
- Intestinal perforation, resulting in peritonitis
- Fistula formation – abnormal connections between bowel loops or to the skin
- Malabsorption syndrome due to chronic intestinal involvement
- Tubercular peritonitis – extensive infection of the abdominal lining
- Sepsis and multi-organ dysfunction in advanced or untreated cases
Delayed diagnosis is a significant concern, as the condition can mimic other diseases and lead to unnecessary surgeries if not identified early.
Diagnosis of Abdominal Tuberculosis
Abdominal TB diagnosis relies on clinical suspicion, especially in endemic areas, supported by a mix of tests:
(1) Blood Tests:
ESR: Often elevated due to chronic inflammation
Hemoglobin: May show anemia of chronic disease
Mantoux Test: Suggests TB exposure; not specific for active disease
(2) Ultrasound Abdomen:
Non-invasive and may reveal ascites, lymphadenopathy, or bowel thickening; useful for guiding biopsies.
(3) CT Scan Abdomen
Offers detailed imaging of thickened bowel loops, necrotic nodes, and peritoneal changes. Aids strong radiological suspicion.
(4) Ascitic Fluid Analysis:
Straw-colored fluid with high protein and lymphocytes
ADA >35–40 IU/L suggests TB
Can be tested for AFB, culture, or GeneXpert
(5) Endoscopy/Colonoscopy
Useful for suspected ileocecal TB; allows direct visualization and biopsy of ulcers or strictures.
Laparoscopy:
Minimally invasive way to view peritoneal tubercles, adhesions, and collect biopsy when imaging is inconclusive.Histopathology:
Gold standard. Shows caseating granulomas, Langhans giant cells, or AFB in tissue samples.GeneXpert MTB/RIF:
Rapid test detecting TB DNA and rifampicin resistance from tissue or fluid; high sensitivity in extrapulmonary TB.
Treatment of Abdominal Tuberculosis
Abdominal TB is treated with a standard anti-tubercular therapy (ATT) regimen, similar to pulmonary TB. The treatment duration typically spans 6–9 months, but may be extended in complicated or resistant cases.
Standard treatment includes:
- Intensive phase (2 months): Isoniazid, Rifampicin, Pyrazinamide, and Ethambutol
- Continuation phase (4–7 months): Isoniazid and Rifampicin
Patients are monitored closely for drug tolerance, adherence, and response to therapy. Nutritional support and treatment of anemia or electrolyte imbalances may also be required.
Surgical intervention
It maybe necessary in cases with:
- Intestinal obstruction
- Perforation
- Persistent abscess or fistula
- Diagnostic uncertainty mimicking malignancy
Lifestyle and Supportive Measures
- Adequate nutrition to combat malnutrition and promote recovery
- Hydration support in cases with ascites or bowel disturbance
- Avoidance of self-medication and over-the-counter antibiotics
- Adherence to treatment is critical to prevent resistance and relapse
- Routine follow-up with a gastroenterologist to monitor progress and manage side effects.
If you’re experiencing chronic abdominal symptoms, especially in the presence of risk factors like TB exposure or weakened immunity, seek medical attention promptly. With early diagnosis and appropriate treatment,abdominal tuberculosis can be cured effectively and complications can be avoided.
Why Choose Us?
Contact Us

