Get Care
Alcoholic Liver Disease
What is Alcoholic Liver Disease (ALD)?
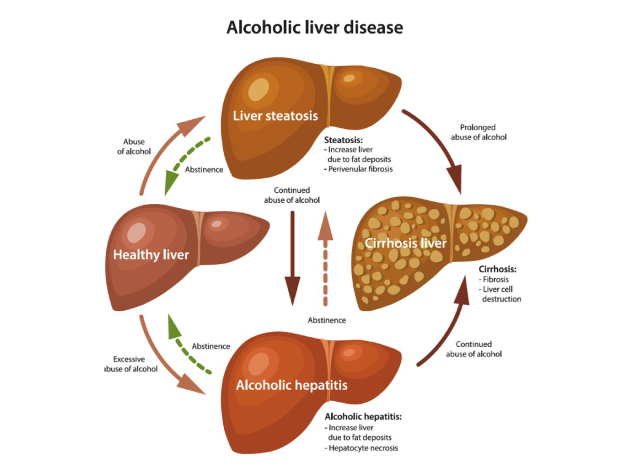
Alcoholic Liver Disease (ALD) refers to a spectrum of liver disorders caused by chronic, excessive alcohol consumption. The liver plays a crucial role in detoxifying alcohol, but over time, continuous alcohol intake can overwhelm its ability to regenerate, leading to progressive liver damage. ALD typically progresses through three stages: fatty liver (steatosis), alcoholic hepatitis, and cirrhosis. Early intervention, especially complete cessation of alcohol, can reverse damage in early stages, but advanced disease may be life-threatening and require specialized interventions.
What are the causes of alcoholic liver diseases?
Chronic Alcohol Use
Long-term alcohol consumption leads to the buildup of toxic metabolites like acetaldehyde, damaging liver cells. Men consuming >40–60g/day and women >20–30g/day are at high risk. Binge drinking also contributes to acute liver injury.
Acetaldehyde Toxicity
Acetaldehyde, a byproduct of alcohol metabolism, causes direct liver cell injury, triggers inflammation, and promotes fibrosis by stimulating collagen production.
Oxidative Stress
Alcohol metabolism creates free radicals (ROS), damaging liver cell structures and impairing mitochondrial function. This oxidative stress contributes to hepatitis and fibrosis.
Fatty Liver (Steatosis)
Alcohol disrupts fat metabolism, causing fat to accumulate in liver cells. This earliest ALD stage is often reversible but sets the stage for more serious damage.
Immune Response
Damaged liver cells activate immune reactions, releasing cytokines and attracting inflammatory cells. This escalates liver inflammation, especially in alcoholic hepatitis.
Nutritional Deficiencies
Alcoholics often lack vital nutrients like vitamins B1, B6, B12, folate, and zinc, weakening liver repair mechanisms and accelerating disease progression.
Genetic & Gender Factors
Some people have genetic variations affecting alcohol metabolism, increasing vulnerability. Women are more susceptible to ALD due to lower alcohol breakdown capacity and hormonal factors.
What are the Symptoms of Alcoholic Liver Disease?
Symptoms of Alcoholic Liver Disease vary based on the stage of liver damage and may initially be mild or absent. As the disease progresses, symptoms become more prominent and potentially life-threatening.
(1) Early Symptoms (Fatty Liver)
Fatigue: A persistent feeling of tiredness or lack of energy, often the first noticeable sign.
Loss of appetite: Decreased interest in eating, which may contribute to weight loss.
Right upper abdominal discomfort: A dull ache or fullness beneath the rib cage on the right side due to liver enlargement.
Nausea and bloating: Mild digestive issues may accompany early liver fat accumulation.
(2) Alcoholic Hepatitis
Jaundice: Yellowing of the skin and eyes caused by increased bilirubin due to impaired liver function.
Fever: A low-grade fever due to inflammation in the liver.
Pain and tenderness in the upper right abdomen: The liver becomes swollen and sensitive to touch.
Vomiting and nausea: More pronounced, often with loss of appetite.
Swelling in the abdomen (ascites): Fluid accumulation due to increased portal pressure and decreased protein production.
Muscle weakness and weight loss: Resulting from malnutrition and liver dysfunction.
(3) Advanced Cirrhosis
Hepatic encephalopathy: Confusion, irritability, drowsiness, or even coma due to toxin buildup in the brain.
Easy bruising or bleeding: The liver’s reduced ability to produce clotting factors leads to frequent nosebleeds, gum bleeding, or bruises.
Swollen legs and ankles (edema): Due to poor protein synthesis and fluid retention.
Spider angiomas: Small, spider-like blood vessels visible on the skin, typically on the upper chest and face.
Redness of the palms (palmar erythema): Caused by changes in hormone metabolism.
Dark urine and pale stools: Indicating poor bile flow due to liver dysfunction.
Gastrointestinal bleeding: Vomiting blood or passing black, tarry stools due to varices in the esophagus or stomach.
What are the Diagnostic Approach?
Diagnosis is based on clinical history, physical examination, and investigations:
Liver function tests: Elevated AST, ALT, bilirubin; low albumin; prolonged prothrombin time.
Ultrasound abdomen: To detect liver enlargement, fat deposition, or cirrhosis.
Fibroscan: Non-invasive test to measure liver stiffness and assess fibrosis.
CT or MRI scan: To evaluate the liver’s structure and detect complications.
Liver biopsy: Sometimes needed to confirm alcoholic hepatitis or rule out other liver diseases.
What are the Complications?
Untreated or progressive ALD can result in serious complications:
Liver failure: Complete loss of liver function, requiring urgent medical intervention.
Portal hypertension: High pressure in the liver’s blood vessels, leading to fluid leakage and varices.
Ascites: Fluid buildup in the abdomen, often requiring repeated drainage.
Esophageal varices: Swollen veins in the esophagus that can rupture and bleed severely.
Hepatic encephalopathy: Mental decline due to buildup of toxins like ammonia.
Spontaneous bacterial peritonitis (SBP): Infection of the fluid in the abdominal cavity.
Liver cancer (Hepatocellular carcinoma): Cirrhosis increases the risk of developing cancer.
What is the Treatment Approach?
The foundation of ALD treatment is complete and lifelong abstinence from alcohol. Additional therapies depend on the stage of liver disease.
Lifestyle and Supportive Measures
Alcohol cessation: The most critical intervention. Support through de-addiction counseling, behavioral therapy, and medications like naltrexone or acamprosate may help.
Nutritional rehabilitation: High-calorie, high-protein diet with vitamin supplementation—especially thiamine, folate, and B-complex vitamins.
Medical Management
Corticosteroids: Used in selected patients with severe alcoholic hepatitis to reduce liver inflammation.
Pentoxifylline: An alternative in some patients with contraindications to steroids.
Lactulose and rifaximin: To treat hepatic encephalopathy by reducing ammonia levels.
Diuretics (spironolactone, furosemide): To manage ascites and swelling.
Management of Complications
Endoscopy: To detect and treat esophageal varices.
Paracentesis: Drainage of ascitic fluid in cases of discomfort or infection.
Antibiotics: For infections like spontaneous bacterial peritonitis.
Liver Transplant
Considered in patients with end-stage liver failure who meet eligibility criteria and have maintained alcohol abstinence for a minimum duration (typically 6 months).
Why Choose Us?
Contact Us

