Get Care
CA Colon (Colon Cancer)
What is Colon Cancer (CA Colon)?
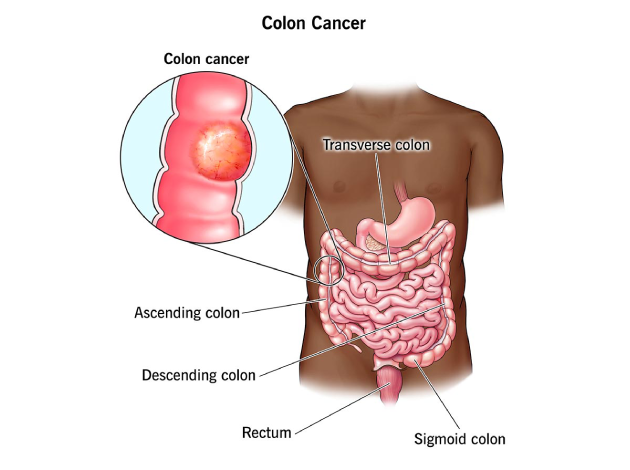
Colon Cancer, also known as colorectal cancer when it involves both the colon and rectum, is a malignant growth that originates in the lining of the large intestine (colon). It typically begins as small, benign clumps of cells called polyps, which may gradually become cancerous over time. Colon cancer is one of the most common gastrointestinal cancers and is highly treatable if detected early.
Colon cancer can affect any part of the colon, and the symptoms may vary based on the location and extent of the tumor. It often develops silently and may remain asymptomatic until it reaches an advanced stage, making routine screening essential.
What Causes Colon Cancer?
Genetic Mutations & Polyps
Most cases begin as adenomatous polyps. Mutations in genes like APC, KRAS, and TP53 drive their progression to cancer. Larger or multiple polyps raise the risk.Chronic Inflammation
Conditions like ulcerative colitis and Crohn’s disease increase risk due to long-term inflammation that damages DNA and triggers abnormal cell growth.Hereditary Syndromes
FAP: Hundreds of polyps form early; almost always leads to cancer without treatment.
Lynch Syndrome: Early-onset cancer caused by mismatch repair gene mutations.
Age
Risk increases after 50 due to accumulated DNA damage and more frequent polyp formation.Lifestyle Factors
Red/processed meats, low fiber, obesity, inactivity, smoking, alcohol, and type 2 diabetes contribute to risk.Personal History
Previous polyps or colon cancer increases the risk of recurrence.
What are the Signs and Symptoms of Colon Cancer?
Symptoms often depend on the location and extent of the tumor. Common symptoms include:
- Change in bowel habits – constipation, diarrhea, or alternating patterns
- Blood in stool (either visible red blood or occult bleeding)
- Abdominal discomfort – cramping, gas, or pain
- Unexplained weight loss
- Weakness or fatigue (often due to anemia)
- Feeling of incomplete bowel evacuation
- Narrow or ribbon-like stools
- In advanced cases: bowel obstruction, perforation, or palpable abdominal mass
What are the Risk Factors for Colon Cancer?
Colon cancer risk increases due to a combination of genetic, lifestyle, and medical factors. Key risk factors include:
Family history: Especially in first-degree relatives or with inherited syndromes like Lynch syndrome or FAP.
Personal history: Previous polyps, colon cancer, or inflammatory bowel diseases (like ulcerative colitis or Crohn’s disease).
Diet: High intake of red/processed meats, low fiber, and high-fat diets.
Lifestyle: Lack of exercise, obesity, smoking, and heavy alcohol use.
Medical conditions: Type 2 diabetes, prior abdominal radiation therapy.
What are the Complications of Colon Cancer?
Colon cancer can lead to several serious complications, especially if not detected and treated early:
Bowel obstruction: Tumors can block the colon, causing severe pain, bloating, constipation, or vomiting.
Bleeding: Chronic bleeding from the tumor may lead to anemia and fatigue.
Metastasis: Cancer can spread to the liver, lungs, lymph nodes, or other organs.
Perforation: A hole in the colon wall may occur, leading to infection or peritonitis (life-threatening inflammation of the abdominal lining).
Fistula formation: Abnormal connections may form between the colon and other organs, like the bladder or skin.
Recurrence: Even after treatment, colon cancer can return, either locally or in distant organs.
What are the Diagnosis of Colon Cancer?
Diagnosing colon cancer involves a combination of clinical evaluation, imaging, and tissue analysis:
Medical History & Physical Exam: Assessment of symptoms, family history, and risk factors, along with a rectal examination.
Colonoscopy: The gold standard test. A flexible tube with a camera is used to examine the colon and remove or biopsy suspicious growths.
Biopsy: Tissue samples taken during colonoscopy are examined under a microscope to confirm cancer.
Blood Tests:
Complete Blood Count (CBC): Checks for anemia due to bleeding.
CEA Test (Carcinoembryonic Antigen): A tumor marker that may be elevated in colon cancer.
Imaging Studies:
CT Scan or MRI: Helps determine the extent of spread (staging) to lymph nodes or other organs.
PET Scan: Sometimes used to detect metastasis or recurrence.
Early diagnosis greatly improves treatment outcomes and survival rates.
What is the Treatment for Colon Cancer?
Treatment depends on the stage, location, and overall health of the patient. It often involves a multidisciplinary approach:
- Surgery: Mainstay treatment for localized colon cancer. Options include:
- Segmental colectomy or hemicolectomy with lymph node removal
- Laparoscopic or open approach
- Chemotherapy: Adjuvant therapy in stage III and high-risk stage II; used in metastatic disease
- Common regimens: FOLFOX (5-FU, leucovorin, oxaliplatin), CAPOX, FOLFIRI
- Targeted therapy: For advanced cases (e.g., bevacizumab, cetuximab)
- Radiotherapy: Rarely used in colon cancer (more common in rectal cancer)
- Palliative care: For advanced or non-resectable cases to improve quality of life
Lifestyle and Supportive Measures
- Diet rich in fiber, fruits, and vegetables
- Regular physical activity
- Avoidance of smoking and excessive alcohol
- Weight management and diabetes control
- Routine colonoscopy screening starting at age 45 or earlier if high-risk
- Genetic counseling and testing for those with family history
Why Choose Us?
Contact Us

