Get Care
Constipation
What is Constipation?
Constipation is a common digestive condition characterized by infrequent, difficult, or painful bowel movements. It is often defined as having fewer than three bowel movements per week, with stools that may be hard, dry, or lumpy. Constipation can also lead to a feeling of incomplete evacuation or excessive straining during bowel movements. While occasional constipation is common, chronic constipation can significantly impact quality of life and may be indicative of underlying health issues.Constipation can affect individuals of all ages and is more common in older adults. It can be classified as primary (idiopathic) when there is no identifiable cause, or secondary when it results from other medical conditions or lifestyle factors.
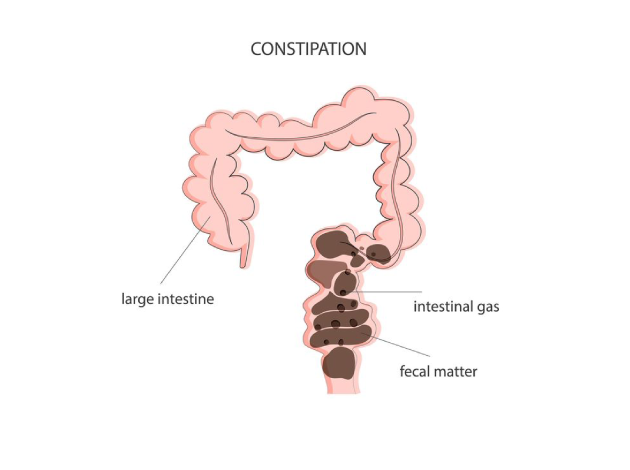
What Causes Constipation?
Constipation can arise from a variety of factors that affect the normal functioning of the digestive system. These include:
(1) Dietary Factors:
- Low Fiber Intake: A diet lacking in fiber-rich foods like fruits, vegetables, and whole grains can lead to constipation. Fiber helps absorb water into the stool and makes it easier to pass.
- Inadequate Fluid Intake: Dehydration is a common cause of constipation, as insufficient fluid intake leads to harder stools that are difficult to pass.
(2) Lack of Physical Activity:
A sedentary lifestyle, especially in older adults, can contribute to constipation by slowing down bowel movements.
(3) Medications:
Certain medications, including painkillers (especially opioids), antacids containing calcium or aluminum, iron supplements, and certain antidepressants, can cause constipation as a side effect.
(4) Medical Conditions:
- Irritable Bowel Syndrome (IBS): IBS is a common gastrointestinal disorder that causes alternating bouts of constipation and diarrhea.
- Hypothyroidism: An underactive thyroid can slow down metabolism and cause constipation.
- Diabetes: Nerve damage related to diabetes can affect the bowel, leading to constipation.
- Neurological Disorders: Conditions like Parkinson’s disease, multiple sclerosis, and stroke can disrupt normal bowel function.
- Pelvic Floor Dysfunction: Weakness or dysfunction in the muscles of the pelvic floor can hinder the ability to pass stool.
- Colorectal Diseases: Conditions such as colorectal cancer or diverticulitis can lead to constipation due to blockage or narrowing of the colon.
(5) Psychological Factors:
- Stress and Anxiety: Emotional stress or anxiety can impact the gut and slow down bowel movements.
- Depression: People with depression may experience constipation as part of the condition or as a side effect of medications used to treat it.
(6) Changes in Routine:
Traveling, pregnancy, or changes in daily habits (e.g., diet, work schedule) can disrupt normal bowel function and lead to constipation.
(7) Aging:
As people age, the digestive system slows down, which can lead to an increased risk of constipation.
What are the Signs and Symptoms of Constipation?
The primary symptom of constipation is difficulty passing stools, but the condition can also present with several other associated signs, including:
- Infrequent Bowel Movements: Fewer than three bowel movements per week.
- Hard or Lumpy Stools: Stools that are dry, hard, and difficult to pass.
- Straining: Excessive straining during bowel movements due to difficulty passing stool.
- Feeling of Incomplete Evacuation: The sensation that the bowel has not fully emptied, even after a bowel movement.
- Abdominal Discomfort: Bloating, cramping, or a feeling of fullness in the abdomen.
- Painful Bowel Movements: Pain or discomfort during the passage of stool.
- Excessive Gas or Flatulence: Accumulation of gas in the intestines can contribute to bloating and discomfort.
What are the Risk Factors for Constipation?
Several factors can increase the risk of developing constipation, including:
- Age: Constipation becomes more common with age, especially in individuals over 65 years.
- Gender: Women are more likely to experience constipation than men, particularly during pregnancy or due to hormonal changes.
- Sedentary Lifestyle: Lack of physical activity can contribute to constipation.
- Poor Diet: A diet low in fiber and high in processed foods can lead to constipation.
- Medications: Certain drugs, such as opioids, antidepressants, and antacids, can cause constipation.
- Medical Conditions: Conditions like diabetes, hypothyroidism, and neurological disorders increase the risk of constipation.
- Stress: Emotional stress can affect bowel movements, leading to constipation.
What are the Complications of Constipation?
While constipation is usually not life-threatening, it can lead to a range of complications if left untreated:
- Hemorrhoids: Chronic straining can lead to the development of hemorrhoids, which are swollen blood vessels in the rectum that cause pain, itching, and bleeding.
- Anal Fissures: Hard stools can cause small tears in the skin around the anus, leading to painful anal fissures.
- Fecal Impaction: In severe cases, the stool can become so hard and dry that it forms a blockage in the colon or rectum, preventing normal bowel movements.
- Rectal Prolapse: Chronic constipation can weaken the muscles and tissues of the rectum, leading to the rectum protruding from the anus.
- Bowel Obstruction: A prolonged blockage of the intestines due to impacted stool may require medical intervention or surgery.
Diagnosis of Constipation
Diagnosis involves identifying the underlying cause through a combination of clinical history, physical examination, and diagnostic testing, especially in chronic or severe cases.
(1) Medical History (Foundational Step)
A comprehensive patient history is critical for identifying possible causes and guiding the diagnostic approach. The doctor may ask about:
- Bowel movement frequency and stool consistency (often assessed using the Bristol Stool Chart)
- Diet and fluid intake, especially fiber
- Physical activity level
- Medication use, including opioids, iron supplements, antacids, or antidepressants
- Symptoms duration, presence of straining, incomplete evacuation, or rectal bleeding
- Any psychological factors, such as stress or anxiety
- Family history of gastrointestinal diseases or colon cancer
(2)Physical Examination
A physical exam, particularly a digital rectal examination (DRE), is often performed to assess:
- Fecal impaction: Hardened stool in the rectum
- Anorectal abnormalities: Hemorrhoids, fissures, or rectal prolapse
- Anal sphincter tone and strength
- Any signs of masses or structural obstruction
DRE is a simple yet informative test that may reveal mechanical or functional problems contributing to constipation.
(3) Blood Tests
Blood tests are used to detect underlying medical conditions that can cause or worsen constipation, including:
- Hypothyroidism: Low thyroid hormone levels can slow bowel motility
- Diabetes Mellitus: Can cause autonomic nerve dysfunction affecting the gut
- Electrolyte imbalances: Low potassium or high calcium can impair bowel movement
- Complete blood count (CBC): May help rule out infection or anemia related to chronic disease.
(4) Imaging Studies
Abdominal X-ray: Shows stool buildup, gas patterns, or signs of obstruction.
CT Scan: Detects tumors, obstructions, inflammation, or perforation—useful in severe or painful cases.
(5) Endoscopic Evaluation
Colonoscopy: For patients ≥45 or with alarming symptoms (e.g., bleeding, weight loss); helps identify polyps, cancer, strictures, or inflammation.
Sigmoidoscopy: Focuses on the lower colon; useful for localized issues or follow-up.
(6) Functional and Motility Tests
Anorectal Manometry: Measures muscle pressure and coordination to detect defecation disorders.
Balloon Expulsion Test: Evaluates the ability to expel stool-like contents.
Colonic Transit Study: Tracks movement of markers to classify constipation as normal, slow transit, or outlet obstruction.
Treatment of Constipation
Treatment of constipation often involves a combination of lifestyle changes, dietary modifications, medications, and in some cases, surgical interventions.
(1) Dietary Changes:
- Increase Fiber Intake: A diet rich in fiber from fruits, vegetables, whole grains, and legumes helps soften the stool and promote regular bowel movements.
- Increase Fluid Intake: Drinking plenty of water helps to prevent dehydration and makes the stool easier to pass.
(2) Exercise
Regular physical activity stimulates bowel movements and helps prevent constipation. Even simple activities like walking can be beneficial.
I. Medications:
- Fiber Supplements: Over-the-counter fiber supplements like psyllium or methylcellulose can help increase stool bulk and promote regularity.
- Laxatives: There are different types of laxatives available, including stool softeners, osmotic laxatives, and stimulant laxatives. These should only be used short-term under medical supervision, as long-term use can lead to dependence.
- Probiotics: Probiotic supplements may help regulate bowel function by balancing gut bacteria
II. Biofeedback Therapy: For patients with pelvic floor dysfunction or other structural issues, biofeedback therapy can help retrain the muscles used in bowel movements.
III.Surgical Intervention: In rare cases, if constipation is caused by a blockage, structural abnormalities, or fecal impaction, surgery may be required to remove the obstruction or correct anatomical issues.
Lifestyle and Supportive Measures
To manage and prevent constipation, individuals can adopt the following habits:
- Establish a Regular Bowel Routine: Setting aside time each day to use the restroom can help train the body for regular bowel movements.
- Avoid Delaying Bowel Movements: Ignoring the urge to have a bowel movement can lead to further constipation.
- Exercise Regularly: Engaging in physical activity helps keep the digestive system functioning well.
Prognosis
In most cases, constipation is manageable with lifestyle changes, dietary modifications, and proper medical treatment. The prognosis for individuals with chronic constipation is generally good, although it may require ongoing management, especially if the underlying cause is a medical condition. If left untreated, chronic constipation can lead to complications such as hemorrhoids, fecal impaction, and bowel obstruction, which can significantly affect quality of life.
Why Choose Us?
Contact Us

