Get Care
Diaphragmatic Hernia
What is Diaphragmatic Hernia?
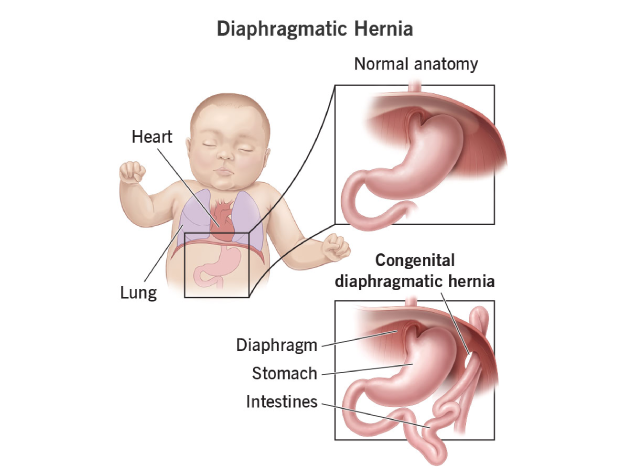
A diaphragmatic hernia is a condition in which an opening or defect in the diaphragm— the muscle that separates the chest cavity from the abdomen—allows abdominal organs, such as the stomach, intestines, or liver, to move into the chest cavity. This abnormal shift of organs can interfere with normal lung development and function, causing respiratory problems and digestive issues. Diaphragmatic hernia can be present at birth (congenital) or develop later in life (acquired), with congenital cases often being more serious due to the risk of affecting lung development in infants.
What are the Causes Diaphragmatic Hernia?
Diaphragmatic hernias are classified as congenital (present at birth) or acquired (develop after birth):
(1) Congenital Diaphragmatic Hernia (CDH)
Occurs when the diaphragm doesn’t fully form during fetal development (usually by 8–10 weeks of pregnancy), leaving a hole that allows abdominal organs to move into the chest, affecting lung development (pulmonary hypoplasia).
Contributing factors:
Genetic mutations or syndromes
Environmental exposures during pregnancy (rare)
Often multifactorial and unclear
Common types:
Bochdalek hernia (posterolateral, most common, usually left-sided)
Morgagni hernia (anteromedial, less common)
(2) Acquired Diaphragmatic Hernia
Develops due to injury or pressure on the diaphragm after birth, allowing abdominal organs to herniate into the chest.
Causes include:
Blunt trauma (e.g., car accidents, falls)
Penetrating injuries (e.g., stab wounds, surgery)
Surgical complications
Increased abdominal pressure from chronic coughing (COPD), obesity, pregnancy, heavy lifting, or constipation
What are the Symptoms of Diaphragmatic Hernia?
Symptoms vary based on whether the hernia is congenital or acquired, and how severe it is.
In Newborns with Congenital Diaphragmatic Hernia:
Respiratory distress: Difficulty or rapid breathing due to underdeveloped lungs.
Cyanosis: Bluish skin, lips, or nails from low oxygen.
Heart murmur: Due to pressure on the heart.
Abdominal distension: Swollen belly from displaced organs.
Decreased breath sounds: Especially on one side, from lung compression.
In Adults with Acquired Diaphragmatic Hernia:
Chest pain and shortness of breath
Abdominal pain, nausea, or vomiting
Heartburn from stomach displacement and acid reflux
What are the Risk Factors for Diaphragmatic Hernia?
The risk factors for diaphragmatic hernia differ between congenital and acquired cases:
Congenital Risk Factors:
- Genetic Factors: A family history of congenital diaphragmatic hernia may increase the risk of the condition.
- Environmental Factors: In some cases, maternal factors like smoking, drug use, or viral infections during pregnancy can contribute to the development of CDH.
- Chromosomal Abnormalities: Conditions like trisomy 18 or 21 (Down syndrome) are associated with a higher incidence of congenital diaphragmatic hernia.
Acquired Risk Factors:
- Trauma: Any injury to the diaphragm, such as from blunt force trauma or surgery, can lead to the development of an acquired hernia.
- Chronic Conditions: Conditions that increase pressure on the diaphragm, such as obesity, chronic coughing, or gastrointestinal disorders, may increase the risk of developing a hernia.
- Age: While CDH is often diagnosed at birth or in early childhood, acquired diaphragmatic hernias are more likely to occur in adults, especially those involved in traumatic accidents or surgeries.
What are the Complications of Diaphragmatic Hernia?
If left untreated, diaphragmatic hernia can lead to severe complications, some of which can be life-threatening. These include:
- Pulmonary Hypoplasia: The underdevelopment of the lungs, especially in congenital diaphragmatic hernia, can lead to chronic respiratory problems and decreased oxygen intake.
- Chronic Respiratory Insufficiency: Due to the compression of the lungs and interference with normal lung function, individuals with diaphragmatic hernia may experience ongoing difficulty breathing.
- Gastrointestinal Obstruction: Displaced abdominal organs can block the normal passage of food or waste, leading to symptoms such as nausea, vomiting, and abdominal pain.
- Strangulation of Organs: In rare cases, a herniated organ can become twisted or pinched, cutting off its blood supply and leading to tissue death (strangulation). This is a medical emergency and requires immediate attention.
- Pulmonary Hypertension: Increased pressure in the lungs due to impaired blood flow, leading to further complications such as heart failure.
- Recurrent Infections: If gastrointestinal contents leak into the chest, it can lead to infections such as pneumonia or pleurisy.
How is Diaphragmatic Hernia Diagnosed?
Diagnosis involves a combination of clinical evaluation and imaging tests:
(1) Chest X-ray
Often the first test done; it may show abdominal organs in the chest, a shifted heart, or underdeveloped lungs (in newborns).
(2) Ultrasound
Used prenatally to detect congenital hernias and assess organ position and lung development. Also helpful postnatally in infants.
(3) CT Scan
Provides detailed images of the diaphragm and herniated organs—ideal for detecting acquired hernias and complications like strangulation.
(4) MRI
Used in complex or prenatal cases to evaluate soft tissues and lung volume, especially when radiation should be avoided.
(5) Endoscopy
Helps assess reflux, gastric obstruction, and the stomach’s position—commonly used in adults with acquired or hiatal hernias.
Treatment Options for Diaphragmatic Hernia
Treatment for diaphragmatic hernia depends on the type (congenital or acquired) and the severity of the condition. The goal is to repair the hernia and alleviate symptoms. Treatment options include:
(1) Surgical Repair:
- Laparoscopic Surgery: In adults with acquired diaphragmatic hernias, minimally invasive laparoscopic surgery is the most common approach to repair the hernia. The surgeon will close the defect in the diaphragm and reposition any displaced organs.
- Open Surgery: In more complex cases or for larger hernias, open surgery may be necessary to access and repair the diaphragm.
- Congenital Repair: For newborns or infants with congenital diaphragmatic hernia, surgery is often required soon after birth. The goal is to close the opening in the diaphragm and reposition the abdominal organs into their correct positions.
(2) Supportive Care:
- Mechanical Ventilation: Infants with severe respiratory distress may require mechanical ventilation to assist with breathing until the surgery can be performed.
- Nutritional Support: Infants with congenital diaphragmatic hernia may need feeding tubes or intravenous fluids to ensure they receive proper nutrition while awaiting surgery.
(3) Post-Surgical Care:
After surgery, patients may require ongoing monitoring and care to ensure that the diaphragm heals properly and that there are no complications such as infection or organ displacement. Long-term follow-up may be necessary for children born with CDH, especially to monitor lung development and respiratory function.
Why Choose Us?
Contact Us

