Get Care
Fatty Liver
What is Fatty Liver?
Fatty liver, also known as hepatic steatosis, is a condition where excess fat builds up in the liver cells. While a small amount of fat in the liver is normal, fat exceeding 5–10% of the liver’s weight is considered abnormal and may lead to inflammation, scarring, and eventually liver damage.
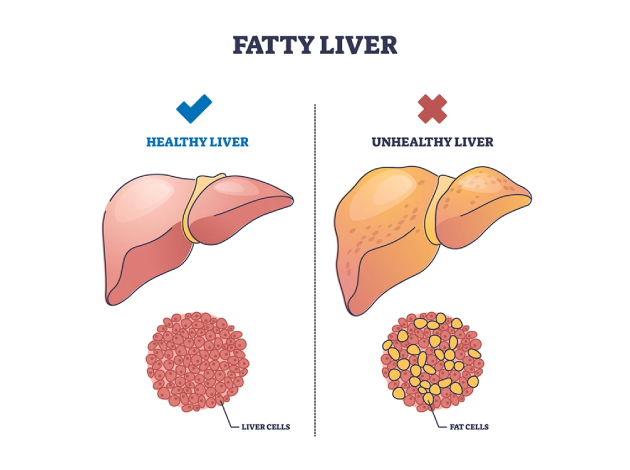
What are the causes of Fatty Liver?
Fatty liver occurs when the liver cannot properly break down and store fats, leading to fat buildup. It can be classified into Non-Alcoholic (NAFLD) and Alcoholic (AFLD) causes.
Non-Alcoholic Causes (NAFLD):
Obesity & Overweight: Excess body fat, especially around the abdomen, promotes fat storage in the liver.
Type 2 Diabetes & Insulin Resistance: High blood sugar and insulin dysfunction lead to fat accumulation.
Dyslipidemia: High triglycerides or low HDL cholesterol disrupt normal fat metabolism.
Metabolic Syndrome: A cluster of conditions including obesity, high BP, and high sugar levels.
Sedentary Lifestyle: Lack of activity encourages weight gain and fat buildup.
PCOS: Associated with insulin resistance and obesity.
Hypothyroidism/Hypopituitarism: Hormonal imbalances slow metabolism and increase fat storage.
Certain Medications: Drugs like steroids and tamoxifen can impair liver function.
Alcoholic Causes (AFLD):
Chronic Alcohol Use: Long-term drinking disrupts fat metabolism and causes liver inflammation.
Binge Drinking: Sudden heavy alcohol intake can acutely stress the liver.
Nutritional Deficiencies: Lack of vitamins like B1 and folate worsens liver repair.
Genetic Factors: Some people are more genetically prone to alcohol-related liver damage.
What are the signs and symptoms of Fatty Liver?
Fatty liver is often asymptomatic, especially in the early stages. When symptoms do appear, they may include:
- Dull pain or discomfort in the right upper abdomen
- Fatigue and low energy levels
- Unexplained weight loss
- Malaise or general feeling of illness
- Loss of appetite
- Abdominal fullness or bloating
In more advanced stages (non-alcoholic steatohepatitis or cirrhosis), symptoms may include:
- Yellowing of the skin or eyes (jaundice)
- Swelling of legs or abdomen (ascites)
- Spider-like blood vessels on the skin
- Confusion or memory issues (hepatic encephalopathy)
- Muscle wasting
- Easy bruising or bleeding
What are the risk factors for Fatty Liver?
Several lifestyle and medical conditions increase the risk of developing fatty liver:
- Obesity (especially abdominal or visceral fat)
- Type 2 diabetes and insulin resistance
- High cholesterol or triglyceride levels
- Sedentary lifestyle
- Poor dietary habits (high sugar and saturated fats)
- Rapid weight loss or starvation diets
- Use of certain drugs (e.g., amiodarone, steroids)
- Genetics and family history
- Obstructive sleep apnea
- Metabolic syndrome
What are the complications of Fatty Liver?
While simple fatty liver may remain benign, progression to non-alcoholic steatohepatitis (NASH) and beyond can lead to serious complications:
- Liver Fibrosis: Scarring of liver tissue due to chronic inflammation.
- Liver Cirrhosis: Permanent liver damage leading to impaired function.
- Liver Failure: Inability of the liver to carry out vital functions.
- Portal Hypertension: Increased pressure in the liver’s blood vessels.
- Esophageal varices: Enlarged veins prone to bleeding.
- Hepatocellular carcinoma (Liver cancer)
- Cardiovascular disease: Leading cause of death in NAFLD patients.
- Cholelithiasis (gallstones): Due to associated metabolic disturbances.
How is Fatty Liver diagnosed?
Fatty liver is often discovered during routine tests or imaging. Diagnosis involves:
(1) Blood Tests
Liver Function Tests (LFTs): Detect elevated liver enzymes (ALT, AST), suggesting inflammation or damage.
Fasting Blood Sugar & HbA1c: Identify diabetes or insulin resistance.
Lipid Profile: Checks cholesterol and triglyceride levels linked to fat buildup.
Thyroid Function: Screens for hypothyroidism, a fatty liver risk factor.
Hepatitis & Autoimmune Markers: Rule out other liver conditions (e.g., Hepatitis B, C, autoimmune hepatitis).
(2) Imaging Studies
Ultrasound: Common, non-invasive test to detect fat in the liver, though not fibrosis.
FibroScan: Measures liver stiffness (fibrosis) and fat content.
MRI/CT Scan: Offers detailed liver imaging; MRI-PDFF is especially accurate for liver fat.
(3) Liver Biopsy
Gold Standard: Confirms NASH and fibrosis severity.
Reserved for unclear cases, persistent abnormal labs, or suspected advanced disease.
Invasive, with minor risk, but highly accurate.
What is the Treatment for Fatty Liver?
There is no specific medication universally approved for fatty liver. The mainstay of treatment lies in lifestyle modification and managing associated conditions.
(1) Lifestyle Modifications
- Weight loss: Target 7–10% reduction in body weight through diet and exercise
- Dietary changes: Avoid sugar-sweetened beverages, refined carbs, saturated fats; increase intake of vegetables, whole grains, lean proteins
- Regular physical activity: At least 30 minutes of moderate-intensity exercise 5 days a week
- Avoid alcohol completely in both NAFLD and AFLD
(2) Medical Management
- Control of diabetes and insulin resistance
- Lipid-lowering drugs (e.g., statins) if necessary
- Vitamin E in select non-diabetic NAFLD patients with biopsy-proven NASH
- Pioglitazone in selected cases (under specialist supervision)
- Manage associated thyroid or metabolic disorders
(3) Surgical/Advanced Interventions
- Bariatric surgery may be considered for obese individuals unresponsive to lifestyle measures
- Liver transplantation for end-stage liver failure due to cirrhosis
Why Choose Us?
Contact Us

