Get Care
Haemorrhoids/Piles
What are Haemorrhoids (Piles)?
Haemorrhoids, commonly known as piles, are swollen blood vessels in the lower part of the rectum and anus. They are a common condition that affects people of all ages, particularly those over the age of 50. Haemorrhoids can occur either inside the rectum (internal) or under the skin around the anus (external). While they are usually not serious, they can cause significant discomfort and pain.Haemorrhoids develop when there is increased pressure on the veins in the rectum and anus, causing them to stretch and swell. This increased pressure may result from factors like constipation, pregnancy, obesity, prolonged sitting, or heavy lifting.
The Types of Haemorrhoids
Haemorrhoids are classified into two main types:
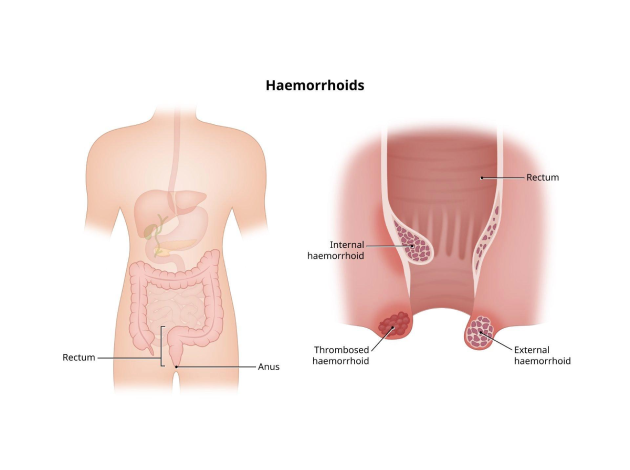
- Internal Haemorrhoids: These occur inside the rectum and are typically not visible. They are usually painless but may cause bleeding during bowel movements.
- External Haemorrhoids: These occur under the skin around the anus. They can cause significant pain, swelling, and itching, and may be visible as a lump or bulge near the anal opening.
What Causes Haemorrhoids?
Haemorrhoids are primarily caused by increased pressure on the veins in the lower rectum. Some common causes include:
- Chronic Constipation: Straining to pass hard stools places excessive pressure on the rectal veins, leading to haemorrhoids.
- Pregnancy: The growing uterus puts pressure on the veins in the rectal area, which can cause haemorrhoids, particularly during labor and delivery.
- Obesity: Extra weight can increase pressure on the pelvic veins, making haemorrhoids more likely to develop.
- Prolonged Sitting: Sitting for long periods, particularly on the toilet, can put pressure on the rectum and anus, increasing the risk of haemorrhoids.
- Heavy Lifting: Frequent lifting of heavy objects can increase intra-abdominal pressure, which may lead to the formation of haemorrhoids.
- Aging: As people age, the tissues that support the veins in the rectum and anus can weaken, making haemorrhoids more common.
- Genetics: A family history of haemorrhoids may increase the likelihood of developing the condition.
What are the Signs and Symptoms of Haemorrhoids?
The symptoms of haemorrhoids can vary depending on whether they are internal or external. Common symptoms include:
- Bleeding: Bright red blood in the stool, on toilet paper, or in the toilet bowl. This is more common with internal haemorrhoids.
- Pain and Discomfort: Particularly with external haemorrhoids, pain and soreness may be felt around the anus, especially during bowel movements or sitting.
- Swelling and Lumps: A visible lump near the anus may be felt in the case of external haemorrhoids. The lump may be tender or painful to the touch.
- Itching and Irritation: The area around the anus may become itchy, irritated, and inflamed, especially with external haemorrhoids.
- Mucus Discharge: A mucus-like discharge from the anus may occur, especially in the case of prolapsed internal haemorrhoids.
In more severe cases, haemorrhoids can lead to prolapse, where internal haemorrhoids slip outside the anus and cannot be pushed back in.
What are the Risk Factors for Haemorrhoids?
Several factors increase the risk of developing haemorrhoids, including:
- Age: Haemorrhoids are more common in people over the age of 50, though they can occur at any age.
- Chronic Constipation or Diarrhea: Both conditions lead to straining during bowel movements, which increases pressure on the rectal veins.
- Pregnancy: Pregnancy increases the risk of haemorrhoids due to the additional pressure exerted by the growing uterus on the pelvic veins.
- Sedentary Lifestyle: Lack of physical activity and prolonged sitting can increase the likelihood of developing haemorrhoids.
- Obesity: Being overweight increases the pressure on the rectal veins, leading to the development of haemorrhoids.
- Genetics: A family history of haemorrhoids can increase the likelihood of developing the condition.
- Heavy Lifting: Frequent lifting of heavy objects can increase abdominal pressure and strain the rectal veins.
What are the Complications of Haemorrhoids?
While haemorrhoids are typically not life-threatening, untreated or poorly managed haemorrhoids can lead to complications:
- Anemia: Persistent bleeding from haemorrhoids can lead to anemia, which results in fatigue, weakness, and shortness of breath.
- Strangulated Haemorrhoid: If a prolapsed internal haemorrhoid becomes trapped outside the anus and its blood supply is cut off, it can become strangulated, causing severe pain and potentially requiring emergency surgery.
- Blood Clots: External haemorrhoids can sometimes develop blood clots, leading to thrombosis. This can cause a painful, hard lump near the anus.
- Infection: In rare cases, external haemorrhoids can become infected, leading to additional pain and swelling.
Diagnosis of Haemorrhoids
Diagnosing hemorrhoids involves a combination of a thorough clinical evaluation, physical examination, and specialized procedures to rule out other possible anorectal conditions.
1. Medical History and Symptom Review
The first step in diagnosing hemorrhoids is a comprehensive medical history, where the doctor will ask about:
- Symptoms such as rectal bleeding (bright red blood), itching, pain, swelling, or a palpable lump
- Bowel habits, including constipation, straining, or prolonged sitting on the toilet
- Any history of hemorrhoids, prior treatments, or surgeries
- Family history of colorectal disease, which may influence further evaluation
- Associated symptoms like weight loss, mucus discharge, or change in stool consistency, which may indicate other gastrointestinal issues
2. Physical Examination
A visual inspection of the anal area is performed with the patient lying in a lateral or lithotomy position. This examination can reveal:
- External hemorrhoids as bluish, swollen lumps near the anal opening
- Prolapsed internal hemorrhoids, which may protrude through the anus during straining
- Signs of thrombosis, where a blood clot causes a firm, painful lump
- Skin irritation, fissures, or infections around the anus.
This initial inspection helps determine whether further diagnostic procedures are needed.
3. Digital Rectal Examination (DRE)
A digital rectal exam is a key part of the assessment:
- The doctor inserts a gloved, lubricated finger into the rectum to feel for internal hemorrhoids, mass lesions, or abnormalities in the anal canal and lower rectum
- This helps assess anal sphincter tone, tenderness, or other potential causes of symptoms like tumors or rectal prolapse
- It provides tactile information that is not visible externally
DRE is a quick, low-risk procedure essential in evaluating internal pathology.
4. Anoscopy
If internal hemorrhoids are suspected, the next step is anoscopy:
- An anoscope, a short, rigid tube with a light source, is gently inserted into the anus
- It provides a direct visual examination of the anal canal and lower rectum
- The doctor can assess:
- The number and size of internal hemorrhoids
- Whether they are bleeding, inflamed, or prolapsing
- The degree of prolapse (graded from I to IV)
- Anoscopy is especially helpful in differentiating hemorrhoids from anal fissures, polyps, or masses
This in-office procedure is generally well tolerated and very effective for internal hemorrhoid diagnosis.
5. Sigmoidoscopy or Colonoscopy
These more comprehensive tests are not routinely performed for straightforward hemorrhoids but may be recommended if:
- The patient is over 45–50 years old
- There is unexplained rectal bleeding
- There are changes in bowel habits (e.g., diarrhea, constipation, stool caliber)
- A family history of colorectal cancer or polyps is present
- Symptoms persist despite treatment
Treatment of Haemorrhoids
The treatment for haemorrhoids depends on the severity of the symptoms. Options include:
Conservative Treatments:
- Dietary Changes: Increasing fiber intake to soften stool and prevent straining.
- Stool Softeners: These can help prevent constipation and ease bowel movements.
- Topical Creams or Ointments: Over-the-counter creams, such as hydrocortisone or witch hazel, can help reduce inflammation, swelling, and discomfort.
- Sitz Baths: Soaking the anal area in warm water several times a day can relieve pain and itching.
- Pain Relief: Over-the-counter pain medications like acetaminophen or ibuprofen can help manage discomfort.
Minimally Invasive Procedures:
- Rubber Band Ligation: A rubber band is placed around the base of internal haemorrhoids to cut off blood flow, causing the haemorrhoid to shrink and fall off.
- Sclerotherapy: A chemical solution is injected into the haemorrhoid to shrink it.
- Infrared Coagulation: This technique uses heat to cause scarring and shrink the haemorrhoid
Surgical Treatment:
- Hemorrhoidectomy: Surgical removal of the haemorrhoid may be necessary for large or prolapsed haemorrhoids that do not respond to other treatments.
- Stapled Hemorrhoidopexy: A procedure in which the haemorrhoids are repositioned and stapled back into place to prevent prolapse.
Postoperative Care:
- After surgery, patients are advised to maintain a high-fiber diet, drink plenty of fluids, and avoid straining during bowel movements.
- Pain management may involve prescribed medications, and patients may be advised to take sitz baths to promote healing.
Lifestyle and Supportive Measures
To prevent or manage haemorrhoids, individuals can adopt the following habits:
- Eat a High-Fiber Diet: Eating fiber-rich foods (fruits, vegetables, whole grains) can prevent constipation and reduce straining during bowel movements.
- Stay Hydrated: Drinking plenty of fluids helps keep stool soft and prevents constipation.
- Exercise Regularly: Regular physical activity can help promote regular bowel movements and prevent constipation.
- Avoid Prolonged Sitting: Avoid sitting for extended periods, especially on the toilet, to reduce pressure on the rectum and anus.
- Don’t Strain: Practice healthy bowel habits by not straining or holding your breath during bowel movements.
Prognosis
With early intervention and proper treatment, most cases of haemorrhoids can be managed effectively. Conservative treatments often provide relief, while surgical options offer long-term solutions for more severe cases. It is important to maintain healthy bowel habits and seek medical advice if symptoms persist or worsen.
Why Choose Us?
Contact Us

