Get Care
Pseudocyst Pancreas
What is a Pseudocyst Pancreas?
A pseudocyst in the pancreas is a fluid-filled sac that forms when pancreatic tissue becomes inflamed, usually after an episode of acute pancreatitis or pancreatic injury. Unlike true cysts, which have a lining made of epithelial cells, pseudocysts are not encapsulated by a defined cell layer, making them less stable and more prone to complications. The fluid inside a pseudocyst typically consists of pancreatic enzymes, water, and tissue debris.
Pseudocysts can vary in size, from small, asymptomatic lesions to large, painful masses that put pressure on nearby organs. In many cases, pseudocysts resolve on their own over time, but others may require medical intervention if they cause complications or do not shrink.
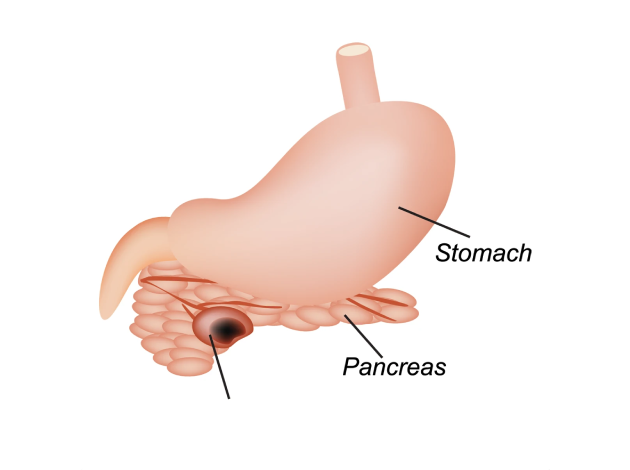
What Causes a Pseudocyst in the Pancreas?
The most common cause of pancreatic pseudocyst is acute pancreatitis. Inflammation during an acute episode leads to leakage of pancreatic fluids, which accumulate and form a fluid-filled sac—eventually encapsulated by fibrous tissue, creating a pseudocyst.
Other contributing causes include:
Chronic Pancreatitis:
Long-standing inflammation, often due to repeated acute episodes or alcohol abuse, leads to scarring and ductal blockage, causing fluid buildup and pseudocyst formation.Pancreatic Trauma:
Blunt or surgical trauma can damage the pancreas and ducts, causing fluid leakage and pseudocyst development—even in those without prior pancreatitis.Pancreatic Duct Obstruction:
Blockages from gallstones, tumors, or strictures prevent pancreatic secretions from draining, leading to pressure buildup and fluid accumulation.Cystic Fibrosis:
This genetic condition causes thick mucus that blocks pancreatic ducts, resulting in chronic inflammation and increased risk of pseudocyst formation.
What Are the Symptoms of a Pancreatic Pseudocyst?
While many pseudocysts remain asymptomatic and resolve on their own, some individuals may experience symptoms, especially if the pseudocyst is large or is causing pressure on surrounding organs. Common symptoms include:
- Abdominal Pain:
The most common symptom of a pancreatic pseudocyst is dull, persistent abdominal pain in the upper left side of the abdomen. The pain can vary in intensity and may worsen after eating or lying down. - Nausea and Vomiting:
As the pseudocyst enlarges, it may cause nausea and vomiting due to pressure on the stomach or other digestive organs. - Bloating and Fullness:
Individuals with larger pseudocysts may feel bloated or full, as the cyst can put pressure on the stomach and intestines. - Jaundice:
In rare cases, the pseudocyst may block the bile duct, leading to a buildup of bile and causing yellowing of the skin and eyes (jaundice). - Fever:
If the pseudocyst becomes infected, fever and chills may develop, signaling the presence of an infection. - Unexplained Weight Loss:
A large pseudocyst that affects digestion may lead to unintentional weight loss due to reduced appetite and malabsorption of nutrients.
How is a Pseudocyst Diagnosed?
Diagnosis of a pancreatic pseudocyst typically involves a combination of physical examination, imaging tests, and lab work to assess the presence of fluid collection and rule out other potential conditions. Key diagnostic methods include:
- Blood Tests:
Elevated amylase and lipase suggest pancreatitis. CBC may show infection; LFTs can indicate bile duct involvement; CRP signals inflammation. While not diagnostic alone, these tests help assess underlying causes and complications. - Abdominal Ultrasound:
A quick, non-invasive first-line tool to detect large fluid-filled cysts. Limited in obese patients or those with bowel gas. Useful for initial screening and guiding drainage procedures. - CT Scan:
The gold standard for evaluating pseudocysts. Offers detailed images of cyst size, location, and complications like infection, rupture, or hemorrhage. Crucial for planning treatment. - MRI / MRCP:
Provides superior soft tissue detail, ideal for complex cases. Helps assess cyst contents and communication with pancreatic ducts. Useful for patients allergic to contrast dyes. - Endoscopic Ultrasound (EUS):
Combines endoscopy and ultrasound for high-resolution internal imaging. Detects small cysts, guides fine-needle aspiration, and aids in endoscopic drainage. - ERCP:
A diagnostic and therapeutic tool for evaluating ductal obstruction or cyst-duct communication. Used selectively due to potential complications like pancreatitis or perforation.
How is a Pancreatic Pseudocyst Treated?
Treatment of a pancreatic pseudocyst depends on its size, location, symptoms, and whether complications such as infection or rupture are present. Common treatment approaches include:
- Observation and Monitoring:
Small, asymptomatic pseudocysts often resolve on their own without the need for treatment. In these cases, doctors may opt for a “watch and wait” approach, with regular imaging to monitor the cyst’s size and potential changes.
- Drainage:
If the pseudocyst is large, symptomatic, or causing complications, drainage may be necessary. There are two main methods of drainage:
- Endoscopic Drainage: A minimally invasive procedure in which a stent is placed through the digestive tract to drain the pseudocyst into the stomach or small intestine.
- Percutaneous Drainage: In this procedure, a needle is inserted through the skin into the pseudocyst to drain the fluid. This is usually done under local anesthesia with imaging guidance.
- Surgery:
In some cases, especially when the pseudocyst is large, persistent, or causing complications, surgical removal may be necessary. The surgeon may drain the pseudocyst or remove it entirely, depending on its characteristics. - Antibiotics:
If the pseudocyst becomes infected, antibiotics may be prescribed to treat the infection. In some cases, drainage may be required to prevent the infection from spreading. - Nutritional Support:
For individuals who experience digestive issues or difficulty eating due to a pseudocyst, nutritional support through a feeding tube or intravenous (IV) nutrition may be necessary until the cyst resolves.
What Are the Complications of a Pseudocyst?
While many pseudocysts resolve without incident, there are potential complications that can arise, especially if left untreated or if the pseudocyst is large. These include:
- Infection:
Infected pseudocysts can lead to severe complications, including sepsis, abscess formation, and organ failure. Infection may require urgent drainage and antibiotic treatment. - Rupture:
A pseudocyst can rupture, leading to the release of pancreatic enzymes into the abdominal cavity. This can cause peritonitis (inflammation of the abdominal lining), which is a life-threatening condition requiring immediate medical intervention. - Bleeding:
In rare cases, a pseudocyst may erode into nearby blood vessels, causing internal bleeding. This can be a serious complication that requires surgical repair. - Compression of Nearby Organs:
Large pseudocysts can put pressure on surrounding organs, such as the stomach, intestines, or bile ducts. This can lead to symptoms like nausea, vomiting, and jaundice. - Chronic Pancreatitis:
Chronic inflammation and repeated episodes of pancreatitis can increase the risk of developing long-term complications like pancreatic insufficiency, which affects digestion and nutrient absorption.
Why Choose Us?
Contact Us

